
Jack Rode’s companion of 28 years, Donna Wendt, died March 13, 2009, at Sunrise Hospital & Medical Center after her windpipe was torn open during the insertion of a breathing tube, causing oxygen to be pumped into her body instead of her lungs. Decorations that Wendt put up in December 2008 still hang.
Sunday, June 27, 2010 | 2 a.m.
Her Life, His Heart
Donna Wendt had her windpipe accidentally torn open at Sunrise Hospital & Medical Center, leaving behind her grieving companion of 28 years, Jack Rode. This is his story, in his own words.
Do No Harm: Hospital Care in Las Vegas
- Prologue: A breakthrough in transparency
- Reporting is the first of its kind in Nevada
- Health care can hurt you
- Accident took her life, his heart
- Fall proves fatal for elderly patient
- Inadequate care, unspeakable pain
- Scarred for life by mistake in surgery
- Where I Stand: Fascination and frustration in reporting on Las Vegas hospital care
- Editorial: Preventing harm
- Health care leaders discuss Sun report’s findings
- St. Rose Dominican Hospitals to post data on quality
- State presses hospitals for full accounting of preventable injuries
Share your stories
Among life’s core assumptions is that hospitals bring healing. But sometimes they bring harm.
Rosie Powell’s surgeon removed a mass from the 74-year-old’s abdomen, thinking it was a cancerous tumor. It was a healthy kidney.
Donna Wendt’s windpipe was torn during insertion of a breathing tube. Oxygen was pumped into her chest cavity instead of her lungs, bloating her. She couldn’t be saved.
Tyrone Bush developed gaping, bone-deep bedsores on his buttocks and heels while recovering from heart surgery. Two years later, he can barely walk.
Morry Janovitz was a day from being released from the hospital when he was found on the floor of his room with a broken neck. He suffered for months from the complications before dying.
They’re not alone.
Over a two-year period — 2008 and 2009 — patients suffered preventable injuries, life-threatening infections or other harm 969 times during their stays in Las Vegas hospitals, an exhaustive Las Vegas Sun investigation has found.
Until now, neither the scale of avoidable incidents nor the hospitals where the harm occurred have been publicly known, in part because hospital lobbyists have resisted the state’s efforts to make the information more public.
Those details are now seeing the light of day.
The Sun has obtained and analyzed a state database in the course of a two-year investigation into the quality of Las Vegas hospitals. The information gleaned from 425,000 inpatient visits tells a story of preventable harm, deadly infections and possible neglect — at a rate of about one injury per day.
Dr. John Santa, director of the Health Ratings Center for the nonprofit organization Consumer Reports, said the events identified by the Sun are important indicators of how hospitals set priorities on patient safety.
“These are events that no one can be proud of,” Santa said. “They aren’t inevitable. They’re preventable. It just involves attention to detail and a willingness to change the culture.”
The Sun’s findings also call into question how well Nevada protects patients from being harmed in hospitals, because it appears the hospitals are failing to report many incidents. State regulators, with whom the Sun’s findings were shared, said they will investigate.
The Sun’s analysis reveals a host of problems encountered by patients, and troubling trends that the hospitals should address. Inpatient hospital records provided by the state show:
• 21 cases in which hospital patients accidentally had foreign objects left in their bodies after surgery — eight at University Medical Center, seven at Sunrise Hospital & Medical Center, three at Valley Hospital Medical Center, two at Southern Hills Hospital & Medical Center and one at Summerlin Hospital Medical Center.
• 79 cases in which a hospital patient developed an advanced-stage pressure sore — an open wound that can hollow out flesh and reach the bone. Sunrise had more than double the rate of any other Las Vegas hospital, with an average of 9 cases per 10,000 inpatient discharges.
• 475 cases of bloodstream infections involving central-line catheters — flexible tubes implanted into main veins to quickly introduce medications. St. Rose Dominican Hospitals, which have perhaps the best reputation for care in Southern Nevada, had by far the highest rates. St. Rose Dominican Hospitals — Siena Campus had more than double the rate of any non-St. Rose hospital in Las Vegas at about 27 per 10,000 inpatient discharges.
• 248 cases in which hospital patients suffered postoperative falls or other trauma. Southern Hills Hospital & Medical Center and North Vista Hospital had almost twice the rate of other Las Vegas hospitals.
The data show 79 instances in the 13 area acute-care hospitals where the harmed patient died. It is impossible to determine based on data whether the hospital-acquired complication contributed to the deaths.
All but one hospital refused to be interviewed to discuss these findings.
The numbers beg for comparison with other regions, but because there are no standardized public reporting methods, it is not possible to make such comparisons.
The federal Centers for Disease Control and Prevention tracks cases nationally of hospital-acquired infections and injuries, but no hospital-specific data are available for public review. Likewise, the Centers for Medicare & Medicaid Services, the government’s insurance payer, tracks such cases, but doesn’t make the information available to the public.

Tyrone Bush and his wife Martha sits in the waiting room in their lawyer's office in downtown Las Vegas Friday, June 11, 2010. In September 2008, Bush had a quadruple heart bypass operation at Desert Springs Hospital Medical Center. The operation was successful, but he developed severe decubitus ulcers, or bedsores, on his buttocks and heels after not being turned or moved enough in his hospital bed. Two years later, Bush cannot work, the wounds are still healing and still cause him severe pain. The Bush's have filed a lawsuit against Desert Springs.
Santa said trying to compare results by state or by hospital leads to “tower of Babel” confusion because so many different measures are used.
In fact, he said, comparing the numbers with other hospitals or regions misses the point. “An argument can be made that anything other than zero is unacceptable.”
But against other national benchmarks, Las Vegas hospitals fare poorly. The Sun found they have higher than expected rates of accidental punctures and lacerations, blood clots and deadly blood infections. Hospital insiders tell the Sun that a dangerous culture of mediocrity has become the status quo. Profits, they say, come before patients. When it comes to staffing, some hospitals try to get by with less.
The incidents of harm identified by the Sun should not happen.
Bedsores are almost always preventable, according to the Institute on Healthcare Improvement, a national nonprofit organization committed to improving patient care. The presence of severe bedsores suggests patients are not receiving proper assessment and care.
Similarly, central-line infections can be prevented with good hand hygiene, daily monitoring of the intravenous catheters and prompt removal when they’re no longer necessary. Researchers famously almost eliminated them from 100 intensive care units in Michigan and their methods are being adopted nationwide.
And a surgery unit at MD Anderson Cancer Center in Houston reduced falls by 75 percent in nine months through improved fall-risk assessment and providing assistance when patients need help most — when they go to the bathroom.
BENEFITS OF TRANSPARENCY
The database tapped by the Sun can be analyzed to identify the hospitals that provide the safest and highest quality care, and those that have repeated incidents of harming patients — making it a potentially powerful tool in deciding where to seek care.
“The more transparency there is the better, (so) consumers can choose their health care facilities,” said Assemblywoman Sheila Leslie, D-Reno, an advocate for improving health care. Such information also benefits insurance companies, which “want to send their insureds to the best possible facility,” she said.
In October 2008, Medicare stopped reimbursing hospitals for preventable “hospital-acquired conditions,” another name for the events identified by the Sun. (The Sun followed Medicare’s lead in determining how to cull the incidents of patient harm from the billing data.)
Medicare’s move addressed the perverse incentive facilities have to not correct harm done to patients: Most insurance companies pay them to treat the hospital-acquired conditions. The injuries can be moneymakers.
Leslie Johnstone, executive director of the Health Services Coalition, which is made up of 24 self-insured health plans in Nevada that cover 260,000 people, said she will study the Sun’s report for trends in poor care at particular facilities or hospital chains. That analysis could prompt insurance payers to direct patients to hospitals with the best care or refuse to pay for ongoing complications that are caused by the facilities, Johnstone said.
The insurance companies have been pushing hospitals to improve. Coalition members could take Medicare’s approach — not pay — if hospital harm can be verified. “That would be a strong argument for why the payment should not be made,” Johnstone said.
FIGHTING TRANSPARENCY
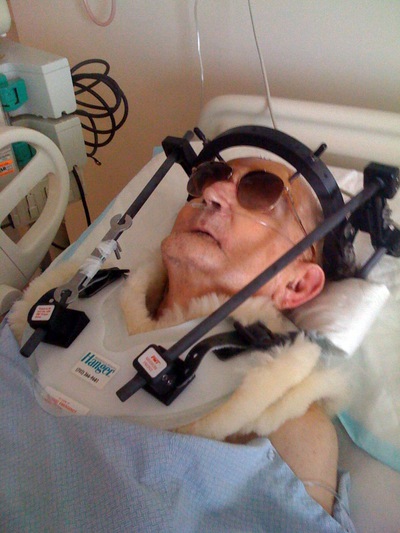
A courtesy photo of Morry Janovitz taken by his wife Pamela after his first fall in Spring Valley Hospital. In late 2008, then 82-year-old Morry Janovitz was admitted Spring Valley Hospital for pneumonia, and the day before he was scheduled to be discharged, he was found on the floor of his hospital room, his neck broken and forehead gashed. Two weeks later he was found on the floor again, this time with just a bruised elbow. Janovitz died from complications three months later.
In 2007, lawmakers passed a bill requiring the state to report, by facility, incidents that harm patients. The state has been conducting the same analysis as the Sun, using the same data and methods. The mandate was for the information to be posted on a website so consumers can compare hospital quality.
According to sources, the state’s effort is yielding the same findings as the Sun’s.
Implementing the legislation has been beset by inaccurate reporting by the hospitals, particularly University Medical Center, as well as budget cuts.
Because of the fiscal crunch, the Health Services Coalition has helped finance the state’s project.
The hospitals have argued that the information should only be published as a statewide total, not by facility.
Chuck Duarte, administrator of Nevada’s Health Care Financing and Policy Division, wrote about the tension in an e-mail Oct. 14 to his supervisor. He reported that Bill Welch, president of the Nevada Hospital Association, said that posting the information by individual facility may prompt hospitals to muddy the information to prevent the events from being identified.
Misreporting data would violate state law.
Welch “also suggested it could lead the NHA to file suit against the state as (the hospitals) are very concerned with their tort liability if hospitals are identified,” Duarte wrote in the e-mail.
Welch said in an interview with the Sun that he told Duarte the hospital association would challenge the state, but never mentioned litigation.
When the hospital lobbyists learned the Sun had obtained the data, they complained to the state that the Sun’s analysis had violated federal patient privacy laws. (The information is public record, and state officials said the Sun did not violate privacy laws.)
UNDERREPORTING THE DATA
Hospital lobbyists and Nevada legislators have spent many hours haggling over transparency laws. The resulting legislation does not benefit consumers as much as it could.
Even so, the Sun’s investigation found hospitals may not be living up to their end of the bargain.
In 2002, during the special session of the Legislature to address doctors’ rising malpractice insurance rates, lawmakers created a registry where hospitals would be required to report “sentinel events” — defined by state law as unexpected incidents that cause serious physical injury or the risk thereof. Sentinel events are deemed so significant that, by law, they trigger internal investigations to determine the cause of the problems and corrective plans to prevent similar harm in the future.
At the time, Welch questioned whether medical error reporting was worth the cost. No study shows that mandatory reporting measurably reduces the errors, he said, according to minutes from the legislative session. The reporting risked compromising patient confidentiality and the physician peer review process and would be costly for hospitals and for state regulators tasked with additional oversight, Welch said at the time.
“The hospitals have been resistant to change every step of the way,” said Assembly Speaker Barbara Buckley, a proponent of the sentinel-events legislation.
The intention, she said, was to increase hospital transparency, reduce costs associated with errors and improve the quality of care.
As a result of negotiations between legislators and hospital lobbyists, the only part of the registry that is public is the total number of sentinel events statewide. Hospital-specific breakdowns are not available, rendering the information essentially meaningless to consumers.
The Sun’s analysis of inpatient records suggests some hospitals are not reporting all of their sentinel events.
The 1,363 incidents of statewide hospital-acquired harm identified by the Sun from the 2008 and 2009 data seem to fit Nevada’s definition of sentinel events. Yet during that period Nevada hospitals reported only 402 sentinel events.
The 2009 data, which the state reported more specifically for sentinel events, provides the best comparison with the Sun’s findings from the hospital inpatient data. For that year:
• Hospitals reported only one sentinel event involving an advanced stage decubitus ulcer — a bedsore that becomes a crater surrounded by dead flesh. The Sun found 72.

Rosie Powell sits on her couch inside her home in Henderson Thursday, May 27, 2010. Powell went in for surgery at St. Rose Dominican Hospital's Siena campus on April 4, 2008, and during a procedure to remove a colostomy bag, surgeons removed Powell's right kidney, which they mistook for cancer. A CT scan following the procedure also revealed a hole between sutures at the site of the colostomy takedown, and after three more procedures to repair the leak Powell now has an ileostomy bag on her right side because of the complications. She is too traumatized to return to the doctor to get it removed. It is hard for her to lay down so she has to prop herself up with pillows to sleep.
• Hospitals reported one sentinel event involving central-line bloodstream infections. The Sun identified 336.
• Hospitals reported six sentinel events in which a foreign object was accidentally left in a patient’s body. The Sun identified 17.
None of the hospitals disputed the Sun’s findings. But they argue many of the incidents identified by the Sun don’t rise to the level of a sentinel event. They call them “adverse” events. (An adverse event is usually defined as a hospital-acquired complication that harms patients, but the term has no legal bearing in Nevada.)
Hospital officials appear to have discretion in determining whether a hospital-acquired injury fits the sentinel-event definition of “unexpected” or causing “serious injury” or the risk thereof. Most wouldn’t discuss that issue on the record.
Officials from almost every hospital in Las Vegas refused to be interviewed for this story. Welch said the hospitals were afraid to speak to the Sun because an interview might violate the federal Health Insurance Portability and Accountability Act, better known as HIPAA, which protects patient privacy. Other medical authorities scoffed at that suggestion.
The only hospital executive who would speak to the Sun for this article was Patricia Scott, vice president of quality for Iasis Healthcare Corp., owner of North Vista Hospital.
Scott said each medical record must be examined before conclusions can be drawn about whether an incident should be reported as a sentinel event. Hospitals take into consideration the course of the patient’s illness and condition, for instance, before determining whether an adverse event was unexpected, she said.
Leslie, the primary author of the state’s sentinel events definition in 2002, said the events identified by the Sun appear to be sentinel events and should be reported as such.
Buckley said, “The hospitals need to explain what happened and then they need to correct the data.”
The state has had no mechanism to determine whether hospitals have been accurately reporting sentinel events. Regulators have trusted the hospitals to do what’s best for patients.
That’s about to change.
As a result of the Sun’s investigation, Richard Whitley, administrator of the Nevada State Health Division, which licenses hospitals and investigates complaints against them, said he would ask hospital administrators to report any previously undisclosed sentinel events. State investigators will then pull medical records to determine the accuracy of each facility’s sentinel events reporting, he said. Nevada can fine hospitals for inaccurate reporting of sentinel events.
In addition, the Health Division will start its own analysis of the same inpatient data examined by the Sun to supplement its own investigations, Whitley said
“Since the Las Vegas Sun identified this analysis of data, we are certainly going to make use of it as well,” Whitley said. “It’s all about improving the quality of health care.”




Join the Discussion:
Check this out for a full explanation of our conversion to the LiveFyre commenting system and instructions on how to sign up for an account.
Full comments policy