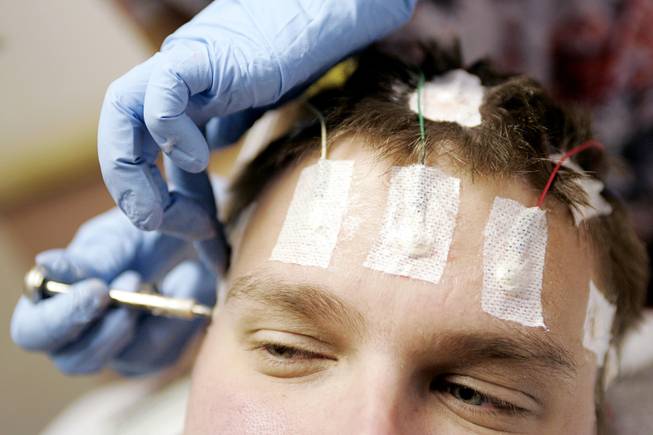
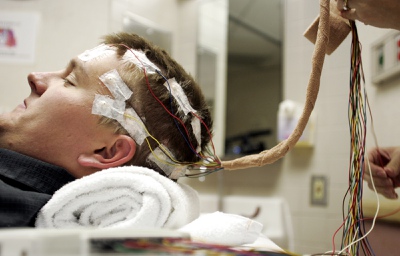
Chris Stones is fitted with 21 electrodes on his head at Sunrise Hospital & Medical Center Monday, October 13, 2008. The electrodes will monitor Stones’ brain activity for several days, and his seizures will be induced to more accurately find the part of his brain where the seizures come from.
Sunday, Oct. 4, 2009 | 2 a.m.
A Hope for Help
Epilepsy has affected Chris Stones' social life, employment and, last year, a seizure he experienced caused a pair of car accidents he cannot remember. He was losing hope that he would find treatment that could help his seizures. Until he met Dr. Samir Bangalore, a neurologist at Sunrise Hospital & Medical Center. He had no idea Bangalore would give him what had eluded him his entire life: Hope.
Chris Stones accelerated his Mazda from a stoplight, faded to the right, bounced off a curb and sideswiped a car in the center lane, causing it to bump into another vehicle.
And he didn’t know it.
When his brain finally kicked in, he noticed that his car was swaying and the front fender was bent. He wondered if he had been the victim of a hit and run.
He pulled over at a gas station and called police.
As they arrived, so did a witness who had also called 911 and was now giving an account. That’s when it sunk in for Stones that he was solely responsible for what had happened.
He told the police he had no memory of what had happened on that September day in 2008. They treated him as if he was on drugs or alcohol — conducting a field sobriety test, yelling at him, shoving him against the car and slapping on handcuffs.
I have epilepsy, he explained in a panic. It causes seizures. What happened was beyond my control.
Stones called his father and stepmother, who came to the scene and vouched for his medical condition. He was given a ticket. He would lose his license for 90 days.
If Stones had been living in ancient times, his epilepsy would have been considered a prophetic power, or a curse. In the Middle Ages, he would have been persecuted and tortured as a witch, or priests would have been summoned to exorcise him of his demons.
Even in 20th century United States, people like Stones could be sterilized, banned from marrying or denied entry into restaurants, theaters and other public places.
And today, if Stones lived in other parts of the world, his seizures would be considered paranormal.
Unfortunately for Stones, epilepsy had become normal.
And after the accident, he’d had enough.
Hopeless, despondent and wracked with guilt over the accident, he reached for his wallet and pulled out a business card that had been given to him several months before for Dr. Samir Bangalore, neurologist, Sunrise Hospital & Medical Center.
He had no idea Bangalore was the only doctor in the state who could provide what had eluded him his entire life: hope.
Sunrise Hospital & Medical Center
•••
Stones’ mother, Kay Spencer, remembers his first seizure. The family was living in Mobile, Ala., and Stones was 6 months old. One night, as he slept between his parents, his body began convulsing. When she picked him up, his tiny body gripped her with spasms so powerful it felt like a man giving her a bear hug.
Stones wasn’t diagnosed with epilepsy at the time but was put on anti-seizure drugs until he was 7, when doctors thought the seizures had stopped. Stones now believes he had more seizures, but they stopped short of convulsions. He suffered from blurred vision and headaches, and would stare mindlessly into space, but those symptoms were not dramatic.
The epilepsy diagnosis came when he was 14. The family was making tacos when Stones thrust his hand into a hot skillet of ground beef, grabbed a handful and shoved it into his mouth. He had a faraway look in his eyes and his skin took on a gray pallor. When he came to his senses seconds later, he saw that his hands were blistered and taco meat was on the counter, but he didn’t know what he had done.
His mom, dad and brother stared at him, dumbfounded.
“You had a seizure,” his mom said.
At the time the family was living in Montana and a neurologist there diagnosed Stones with epilepsy. Stones feared what others would think. His mom says Stones allowed epilepsy to define him, and he carefully structured his life to keep the condition secret. He avoided parties because alcohol — if only from a spiked drink — would cause a seizure. He went to bed early, watched his diet, avoided certain frenetic movies that could trigger a seizure. He kept the secret.
As Stones matured he came to grips with letting people know about his epilepsy, and today, at 27, he says he’s not ashamed of the condition.
But that doesn’t remove the problems associated with the seizures.
No one knew about Stones’ epilepsy when he started dealing cards and roulette at the Suncoast in 2005. Over the years he estimates he’s had dozens of seizures on the job. Often, he sensed them coming. He would feel numbness in his hands or blurred vision for a few seconds before they started and would pretend to stumble, timing a drop of the cards or roulette ball onto the ground with the strike of the seizure. That allowed him to go to the floor, out of sight, while his brain misfired, and resume the game seconds after it passed. His co-workers and pit bosses dismissed these rare incidents as mishaps.
In time, the seizures become too severe to hide — staring into space, twitching his arms, cards flying onto the floor, drooling, vomiting. They were especially common when he worked the swing shift, which made it difficult to sleep.
Once his condition was known, Stones said, Suncoast management, his co-workers and casino guests were exceptionally supportive. Company policy was not as accommodating: It dictated that he be carried off the floor in a wheelchair. The seizures were embarrassing and heightened his anxiety.
The car accident was the final straw. Something had to be done.
• • •
Seizures start with a spark of electrical activity in the brain that spreads out of control like an electrical storm. Why that happens isn’t fully understood, but it may be related to an injury or genetics. Many seizures are barely noticeable to an observer. Whole-body convulsions — “grand mal seizures” — are the most extreme variety and are less common. Stones has had only four of those in his lifetime.
Seizures come in three stages. Warning signs last seconds and might include tingling, racing thoughts or blurred vision. The seizure itself could be nothing more than spacing out, an out-of-body feeling, or movement of the jaw and fluttering eyelids. The aftermath might include memory loss, feelings of shame, embarrassment or nausea.
A person is diagnosed with epilepsy when he has had at least two seizures not caused by a known medical factor. Epilepsy afflicts about 3 million Americans, but it’s often misdiagnosed. Sunrise has monitored about 400 people — many of whom were on anti-seizure medicines for years — and found that only 20 were epileptics.
Non-epileptic seizures can be caused by a psychological problem known as “conversion disorder,” in which a person converts a particular stress to a physical manifestation — such as, for one patient at Sunrise, the emotional response to a song from “Phantom of the Opera.”
In other cases, epileptic seizures can be a reflexive reaction to a particular external stimulation. Flashing lights and hyperventilation are the most common triggers, but in one instance, a patient had full-body convulsions caused by showering. In a case cited in medical books, a patient’s reflexive seizures were activated by the music of Jamaican-born rapper Sean Paul.
Sunrise works to remove non-epileptics from medications that have harmful side effects and refer them to psychiatric care.
• • •
Stones had suffered from epilepsy his entire life, but the September 2008 crash was the first time a seizure had caused a car accident. It came at a time when he was particularly struggling with epilepsy. His patience had run out with local doctors. His anti-seizure medications had stopped working. The seizures were striking with abandon during his shifts at the Suncoast. Usually the anxiety of wondering when and where they would strike was worse than the symptoms themselves.

Chris Stones sets up his table with floor supervisor Ariel Leon, left, after returning to work as a dealer at the Suncoast Casino on Friday, September 4, 2009. Stones' craniectomy was apparently successful in removing the part of his brain that was causing seizures. Stones has not had a seizure since his final surgery over six weeks ago.
Stones’ previous neurologist had moved away — not that he missed him. Every appointment took five minutes. The doctor would test his eyes, his reflexes, have him walk in a line, and then write a new prescription.
What is the point of me coming here? Stones would wonder.
Two days after the crash, Stones stood in the parking lot of the Suncoast with his phone in his hand. Epilepsy ruled his life. It dictated his diet, social habits and sleep schedule. The medication made him fall asleep at work. He delayed dating because he didn’t want to bring the stress of the condition into his love life.
The cumulative hopelessness and anxiety of epilepsy put him into such a depression that his mother said she worried he would kill himself.
His stepmother had given him Bangalore’s card months earlier. A friend had passed it along to her. Maybe he could help, she had said.
Tears in his eyes, he dialed Bangalore’s number.
The neurologist, Stones would learn, is the star of a new epilepsy program at the Nevada Neurosciences Institute at Sunrise Hospital, which provides comprehensive care for epileptic adults, including surgery to remove the parts of a patient’s brain that spark seizures.
Bangalore, who graduated from medical school in 2002, was involved in about two dozen such brain surgeries during his epilepsy fellowship. The surgery has been performed for decades elsewhere, but, true to the underdeveloped nature of health care in Nevada, wasn’t available here until he came to Sunrise to start its program in 2007.
Bangalore wasn’t like the clinical and hurried doctors Stones had seen previously. Bangalore is relaxed and easygoing, with an engaging bedside manner, consistent with his personal life, in which he writes silly poems to his wife and lets loose at karaoke restaurants. He likes it when patients ask questions.
Bangalore also offered expertise that was new to Stones. Bangalore, an Indian who was born and raised in Chicago, was groomed to become a doctor. His mother was a librarian and his father was a researcher at the University of Chicago. After school, Bangalore was a “lab rat,” hanging out with his father at his research facility.
At the Illinois Mathematics and Science Academy — Bangalore jokes that the high school should be called the “Ultimate Nerd Academy” — he competed on the math and debate teams. Ask him what sports he played and he mentions ping-pong.
But neurology requires more careful thought than the quick reactions required at a ping-pong table, and Bangalore is, if nothing else, patient. He and his wife spent 18 months renovating their new Las Vegas home before moving in.
After their first meeting, Bangalore believed Stones would be excellent candidate for surgery. Stones was maxed out on three anti-seizure medications, which sedated him and contributed to his depression, but did not stop the seizures.
Most epileptics can be seizure-free through the use of a single medication, Bangalore said. But about one in four epileptics will not be seizure free on any combination of drugs.
Before surgery could be considered, Bangalore needed to identify where the seizures are conceived in the brain and then ensure that a surgical option would not disable the patient.
For all the doctors Stones had seen, not one had mentioned that surgery could cure his epilepsy. Stones was on board. It didn’t matter how much it cost, how long it took or how much it hurt. The new hope lightened the weight of his depression. His mother remembers the hope in his voice when he called her to tell her about the appointment: “Mom, I met this doctor and I think he can help me!”
His company’s health insurance promised to cover the work, but Stones said he would pay it off in installments if it did not. If all went according to plan, the process would culminate with what Stones described to his mother as cutting open his skull and “scooping out” the diseased part of his brain that caused the seizures.
For Bangalore, the first order of business was to observe and record Stones’ seizures in a clinical setting to precisely map the electrical activity. He had to ensure the misfires didn’t stem from a portion of his brain that controlled other important abilities, such as memory or speech.
Bangalore would have to induce the seizures.
• • •
At Sunrise, four rooms are dedicated to epilepsy surveillance, where patients are withdrawn from their medication, deprived of sleep and otherwise prompted to have seizures. A month after the car accident, Stones spent a week at Sunrise withdrawn from his medication, reading, watching TV, staving off boredom, waiting for seizures to strike.
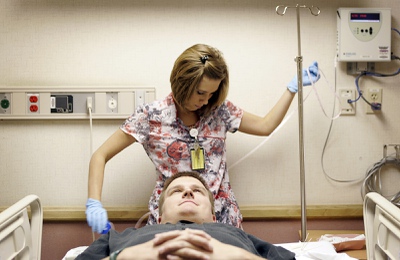
Amber Curl, a registered electroencephalographic and evoked potential technologist at Sunrise Hospital & Medical Center, gets ready to fit 21 electrodes onto Chris Stones head Monday, October 13, 2008. The electrodes will monitor Stones' brain activity, and his seizures will be induced to more accurately find the part of his brain where the seizures come from.
When the seizures came — five of them, eventually — electrodes glued to the outside of his head captured the electrical activity in his brain and transmitted them to an electroencephalography (EEG) machine. Their physical manifestations were captured on video.
Typical of Stones’ seizures was the one that struck at about 11 p.m. Oct. 13. The EEG stylus went from wavy lines to scribbles on the part of the page that represented the frontal and temporal lobes — the area of his brain above and in front of his left ear.
At the same time Stones’ body was in similar disarray. At 6-foot-2 and about 240 pounds, he nearly fills the hospital bed, which has padded rails in case the seizures become violent. When the seizure strikes, he turns from the TV and looks around the room in confusion. His left wrist extends at arm’s length, and he appears to examine his left hand, perplexed. His head turns to the left, his shoulder flexes involuntarily and he vomits in his mouth. As the seizure concludes, Stones looks at both hands, bewildered, and resumes watching TV. The episode lasts about a minute.
Stones’ subsequent seizures at Sunrise included similar involuntary ticks. Sometimes his right arm extended; he clenched, unclenched and shook his right fist; flapped his hands, blinked his eyes. Twice he vomited.
As unsettling as the seizures appear to an outsider, Stones doesn’t recall a time he lived without them, so he’s nonplused about them. They don’t cause pain, and the confusion of the events is mitigated by the fact that they are regular occurrences.
The EEG and the videos taken during the monitoring process showed that the seizures were sparked in the left temporal lobe — the area around the temple involved in language and memory. The seizures are not severe in terms of symptoms, Bangalore said, “but it severely affects his life.” And there’s evidence, he said, that they could become increasingly difficult to treat. Stones’ brain was abnormal even when he was not having seizures. Frequent electrical discharges made it especially difficult for the epilepsy to be controlled by medication.
Epilepsy can also be deadly. Some patients die in a little-understood manner reminiscent of Sudden Infant Death Syndrome called Sudden Unexpected Death in Epilepsy. Others can get locked into a nonstop seizure that can be remedied in the hospital only with intravenous medicine.
Locating the epilepsy’s source was promising. Temporal lobe epilepsy is the most treatable by surgery because the problem area usually rests near the surface of the brain, making it easier for a surgeon to access.
Still, there is no guarantee that epilepsy surgery will work. And there could be the risk of brain damage.
• • •
On Dec. 2, after having returned to work, Stones is back at Sunrise, lying flat on an operating room table.
A catheter is laced through his right femoral artery, starting at his groin, guided up through his midsection and into his brain. Doctors are going to shoot a drug through the catheter that will anesthetize, one at a time, the left and right hemispheres of Stones’ brain. While the hemispheres are numbed, Bangalore will perform neurological tests to determine how his language and memory would be affected if he lost part of his left temporal lobe. It’s called the Wada test, named for Dr. Juhn Wada, the physician who first performed it.
Stones is right handed, so Bangalore said there’s a 95 percent chance the left side of his temporal lobe is partially responsible for his ability to speak. The temporal lobe also contributes to a person’s memory, but it was likely, and would be ideal, if both sides of his temporal lobe contributed to memory. That way if part of the left side were removed, the right side could compensate.
Bangalore has Stones raise his arms, hands outstretched, to show when the drugs take effect on his brain. The anesthetic is injected into the right side of his brain and the left arm falls to the table. The EEG flat-lines on the section representing the right hemisphere. Half of his brain is effectively dead.
The test begins.
“Where did you grow up?” Bangalore asks Stones.
“Albuquerque,” Stones replies, naming his birthplace.
The question isn’t important. What is vital is that Stones can understand it and speak with his right temporal lobe disabled. The ability to receive and produce language is apparently nestled in the still-awake left temporal lobe, as expected.
Bangalore pulls out a stack of flashcards and shows them to Stones: sunglasses, toothbrush, screwdriver and dice. Stones names them one at a time, successfully completing the language test.
Then Bangalore performs a memory test. With Stones’ right hemisphere still numb, the doctor shows him 10 objects — a pair of dice, car, baby doll, stuffed ball, cell phone and other common items. Bangalore waits about 10 minutes for the anesthesia to wear off, allowing the right brain to wake up. Then the doctor shows him the same 10 objects, but throws in others that Stones had not seen.
“Did you see the dice before?”
“Yes.”
Did you see this baby doll before?
“Yes.”
“Did you see this comb?”
“No.”
Stones passes the test.
As was expected, his abilities to remember things and to speak are not affected with the right brain disabled. That means they are housed in the temporal lobe region of the left brain — where the epilepsy is rooted.
The catheter that’s running through Stones’ body is backed up a bit and rerouted into a different artery that leads to the left hemisphere of his brain. The anesthetic is injected again, disabling the left brain, and the Wada test is repeated. Stones passes the memory portion. His memory function is indeed located on both sides of the temporal lobe.
With Stones’ left brain still disabled, Bangalore shows him objects and asks him to name them. Stones is unable to form the words. His eyes indicate that he recognizes the objects, but he struggles to open his mouth. He can’t make a sound.
It is confirmed that Stones’ ability to speak is rooted in the left hemisphere of his brain, where the seizures begin. Before the surgery can be performed, Bangalore will have to do more careful mapping of Stones’ brain to make sure his speech will not become disabled.
• • •
Two weeks after the Wada test, a Nevada Highway Patrol officer raps on Stones’ door. She wants to arrest him for a hit and run.
Stones doesn’t know what she is talking about. His car is in the driveway, undamaged. He can’t remember any accident.
But he has a sick feeling the patrolwoman is right. Stones had been given his license back and has been driving himself to work, cautiously and with much anxiety. The first accident had been a fluke, he assumed. Bangalore was monitoring his medications and the seizures were at bay.
But now his worst fear has come true.
The officer, incredulous that Stones claims he didn’t remember, fills in the details.
Two days earlier Stones was driving north on Interstate 15. He was following a taxicab, when he suddenly revved his speed to about 80 mph, running into the cab’s rear bumper. Videos taken by the cab showed Stones backing off, then revving his engine two more times, bumping the cab again and again before the taxi driver pulled out of his way, allowing him to pass. No damage was done to either car, but Stones didn’t slow down. He continued on his way as if nothing had happened.
Which is why the highway patrol officer is at his door.
Stones explains he is epileptic and begs for leniency. The officer settles for leaving a citation for following too closely, hit and run and failure to report an accident to police. Stones would have to answer in court.
Despondent, he swears not to drive again until his epilepsy can be cured. He calls Bangalore.
The drugs have worn off, Stones tells Bangalore. We’ve got to make this happen faster.
• • •
You don’t just watch a craniectomy. You smell it. It’s July 14 and Stones is unconscious on an operating room table at Sunrise Hospital. Wisps of smoke rise from his head as incisions are cauterized to slow the bleeding.
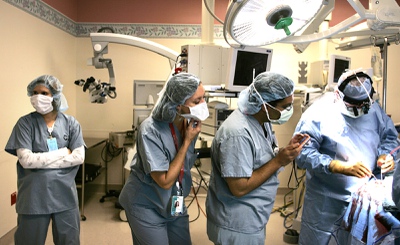
Epilepsy techs Amber Curl, from left, and Karolyn Witcher, with neurologist Dr. Samir Bangalore, watch as neurosurgeon Dr. Stuart Kaplan performs Chris Stones' first brain surgery at Sunrise Hospital & Medical Center on Tuesday, July 14, 2009. Stones will be fitted with electrodes that attach directly to his brain, where his seizures can be more accurately pinpointed.
Stones’ head is tilted to the right and the whine of a saw fills the room. Bone dust shoots into the air. Neurosurgeon Stuart Kaplan is cutting free an oval of skull, the size of a large potato chip, above Stones’ left temple.
Kaplan removes the skull chip, exposing the brain. The cranial arteries visibly pulsate with each heartbeat beneath the dura mater, the brain’s fabric-like protective sheath.
Next, Bangalore supervises the placement of a panel of about 40 electrodes on the brain. Tucked into the hole in the skull, the electrodes are arranged in a grid on a soft rubber pad that covers the portion of the left temporal lobe that is the epicenter for Stones’ seizures.
The electrodes will allow Bangalore to precisely locate the seizure onset zone and language ability, by repeating the same tests he had performed about a year before in Sunrise’s monitoring room. That means Stones will be without the portion of his skull for a week.
A few days after the craniectomy, Stones is again taken off his medication and deprived of sleep to induce seizures. This time, the electrodes placed directly on the brain give the precise location of the its misfires. By July 20, the location of the genesis of the seizures is mapped. Now Bangalore needs to map the parts of the brain that contain anything related to language. Once he maps the location of both the seizures and language, he can overlay them and oversee the removal of any parts of the brain that cause seizures but do not affect language.
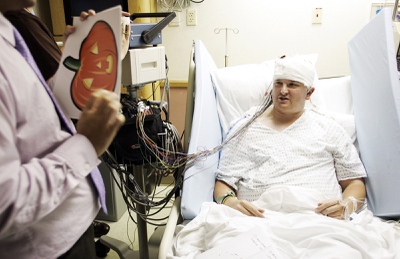
Dr. Samir Bangalore, left, a neurologist who specializes in epilepsy treatment at Sunrise Hospital & Medical Center, performs a test to carefully map the language functions of Chris Stones' brain after his first surgery Monday, July 20, 2009. The test will help determine the exact location of the seizures, and make sure that no essential language or motor functions are stored in that part of the brain, so that the neurosurgeon can remove that part of the brain during a second surgery.
Stones says it’s odd missing part of his skull. When he coughs or sneezes, he says, it feels like his brain is going to fall out of his head.
Stones sits in a hospital bed, wires from the electrodes protruding from his bandaged head. It’s time to map the language. A technician flips a switch that shoots a small dose of electricity to pairs of the electrodes in his brain, disabling for several seconds that part of the brain.
At the instant the brain is zapped, Bangalore shows him a picture of something he would easily recognize: a sailboat, a crocodile, a bear. Naming items is a complex task for the brain because it tests a person’s ability to understand what he is looking at and to say it — reception and expression. If Stones can still name the item in the picture, Bangalore knows it does not control language and can be removed. If zapping the problem area makes it impossible for Stones to speak, then the doctor knows that the portion of brain can’t be removed.
Stones goes mute when eight of the electrode pairs are zapped. Those portions of his brain must remain.
• • •
The next day Stones is back in the Sunrise operating room for his final surgery. He is unconscious. The chip of Stones’ skull, which had been stored in deep freeze by a company in California, is unpacked from dry ice and carried to the operating room table, where, at the end of the operation, it will be reattached with screws.
Bangalore is on hand to advise Kaplan, the neurosurgeon, throughout the procedure, and the doctors are surrounded by about a half dozen nurses and technicians.
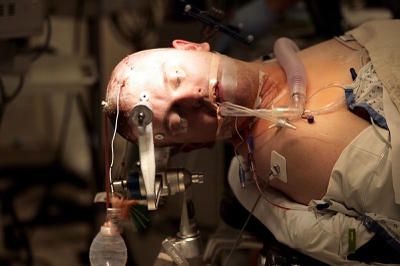
The electrodes that were placed on his brain in the first surgery are seen coming out of Chris Stones' head as he is under anesthetic and being prepared for his second brain surgery, to remove the part of his brain that is causing seizures, at Sunrise Hospital & Medical Center on Tuesday, July 21, 2009.
Bangalore’s brain mapping had determined that the seizure onset zone is on the bottom of Stones’ left temporal lobe. The section that will be removed is about 4 centimeters by 3 centimeters by 3 centimeters — about the size of a thumb — located halfway between the edge of Stones’ left eye and the front side of his ear, at the level of the top of his ear.
The section that will be removed is about 2 centimeters below the part of his brain that controls his ability to process language.
Kaplan uses a scanning probe to map and visualize the brain on a monitor, and at times looks through a microscope as he inches instruments deep into the side of Stones’ head. He is careful to stay almost an inch away from the parts of his brain that control language. The brain feels like soft cheese, so the seizure onset zone is no match for Kaplan’s instruments. He uses a tubular surgical wand to nip it into bits and suck it through a hose and into a biohazard waste container.
The procedure lasts about 45 minutes.
• • •
Today, the only sign that Stones has had brain surgery is a scar, mostly covered with hair, that’s shaped like a large question mark on the left side of his head. They call him “The Riddler” at work, after the Batman villain who has question marks on his costume.

Chris Stones shaves before returns to work, his question mark-shaped scar prominent six weeks after his brain surgery Friday, September 4, 2009. Stones will return to work as a dealer at the Suncoast for the first time after his craniectomy was apparently successful in removing the part of his brain that was causing seizures. Stones has not had a seizure since his final surgery over six weeks ago.
He’s had no more seizures. His insurance company has picked up the cost for all the tests, procedures and surgeries, which the hospital said will typically run between $25,000 and $45,000 depending on the patient. Studies show that upfront costs of epilepsy surgeries are offset by long-term savings. Stones’ monthly medications, for instance, cost about $1,500.
Stones is driving through Eastern Avenue’s stop-and-go traffic on his way to work. It’s been six weeks since he was discharged from Sunrise and he’s on his way to the Suncoast for an 11 a.m. shift.
Going through the operation has changed Stones’ outlook on life, he says as he merges onto the Las Vegas Beltway and accelerates to 60 mph. He never complained in the hospital because he didn’t want to worry his loved ones. But now he says the pain he felt during the 12-hours immediately after the portion of his skull was removed, and again when it was replaced, was the most intense he’s ever felt.
But the process resulted in a freedom he’s never before experienced. How can he worry about a bad day at work when Bangalore and the staff at Sunrise saved his life?
“I was always worried that I was going to hit a car or hit a tree or something else,” Stones said.
It’s too soon to declare Stones cured of epilepsy. Bangalore cautiously describes the seizures as “in remission,” but believes the surgery was successful. He said he’ll keep Stones on medication for up to a year because withdrawing it too quickly has risks. Once the medication’s sedating and mood-altering side effects are gone, it’s possible that Stones’ personality may blossom, he said.
Stones says the operation worked. He’s been seizure free and his friends tell him he’s different: more alert, talkative and engaged. His eyes and shoulders appear more relaxed — he’s no longer bracing for a seizure to strike. His supervisors at work have said he’s quicker at his job. Plus, he’s had many experiences that would have previously induced seizures. He didn’t get a good night of sleep after his first night back at work. The next day he came home from work and forgot to take his seizure medication before falling asleep on the couch.
Before the operation, he certainly would have had seizures if he forgot to take his medication. In the past he would have preempted the problem by calling in sick to work. Not anymore.
“I just laughed about it, got ready for work and left.”
Chris Stones is no longer defined by epilepsy.


Join the Discussion:
Check this out for a full explanation of our conversion to the LiveFyre commenting system and instructions on how to sign up for an account.
Full comments policy