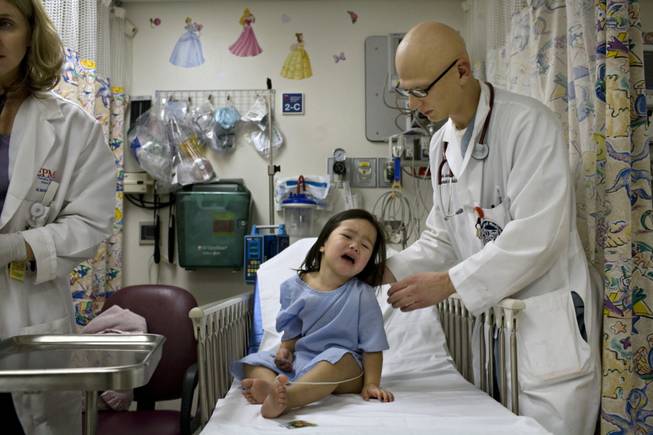
Third-year family medicine resident Dr. Scott Jacobson cares for Kristina Hrubes, 2, Wednesday night in the pediatric emergency unit with attending physician Dr. Michele McKee, left, at University Medical Center.
Thursday, Jan. 14, 2010 | 2 a.m.
Wednesday news conference
Reader poll
Sun Archives
- Rory Reid announces effort to make UMC a teaching hospital (1-13-10)
- Why troubled UMC is in County Commission chairman’s sights (1-5-10)
- Rory Reid’s county rescue plan serves to deflect political opponents’ jabs (1-5-10)
- Commission Chairman Rory Reid unveils cost-cutting plan for county (1-4-09)
- Clark County cost-cutting ideas center on salaries (12-30-09)
People may be puzzled by the plan announced Wednesday to transform University Medical Center into a teaching hospital.
Isn’t it already a teaching hospital?
Yes and no. It’s a hospital that teaches medical students and residents from the University of Nevada School of Medicine, but that does not make it a teaching hospital. Instead, under Clark County’s governance, it’s best known for its mission to take care of the poor and indigent.
If UMC were a teaching hospital, the public might not notice much difference. But academic medicine would be its primary mission, the medical school would have a role in its daily operations and it might be staffed with more faculty instead of community physicians, experts said.
For now, UMC is part teaching hospital and part public hospital, said Brian Brannman, chief operating officer. Some at the hospital are supporters of its graduate medical education — which is focused on internal medicine residency programs — but others pay the mission “lip service,” he said.
Evolving into a teaching hospital means UMC would make a priority of developing the best physicians in Nevada, he said. It would still be charged with taking care of the indigent.
“What it means is that the education mission would become the defining mission,” said Dr. Ole Thienhaus, dean of the School of Medicine.
It’s a difference in focus, said Dr. John Ruckdeschel, director and CEO of Nevada Cancer Institute. Now the hospital is focused on its core mission that revolves around providing care to the indigent, he said. Meeting those obligations has taken a steep financial toll.
The evolution of the mission would require a governance change. Becoming a true teaching hospital allows an academic institution to study the community’s needs and invest in niche needs such as diabetes, with an eye toward research and clinical application that would lift the level of care in the community, Ruckdeschel said.
Brannman said UMC has a good relationship with the school of medicine, but it’s dictated by the relationships between executives at both institutions. If UMC is to be a teaching hospital, the medical school’s role to set direction would need to be cemented into its governance, he said. That would allow joint strategizing about the types of programs to pursue, he said.
Transitioning to a teaching hospital could change the way UMC relates to physicians. The model could take on a lot of different looks, but it might mean that only faculty physicians admit patients, Thienhaus said. Currently at UMC the subspecialists — cardiologists, infectious disease specialists and gastroenterologists, for instance — are physicians who have practices outside the hospital. Before Jan. 1, UMC did not even have an elected chief of staff who was a member of the medical school faculty, Thienhaus said.
Dr. Maurizio Trevisan, executive vice chancellor and CEO of the Health Sciences Center for the Nevada System of Higher Education, said turning UMC into a teaching hospital would mean hiring doctors who teach and do academic research. The transition would be a crucial part of the developing health sciences system and an important way to strengthen the medical school, he said.


Join the Discussion:
Check this out for a full explanation of our conversion to the LiveFyre commenting system and instructions on how to sign up for an account.
Full comments policy