
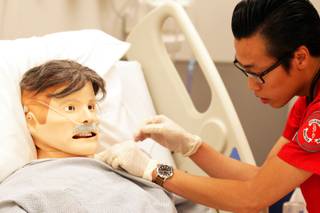
UNLV nursing students run through a simulation with a medical mannequin at the Clinical Simulation Center at UNLV’s Shadow Lane campus in Las Vegas on Thursday, October 4, 2012.
Monday, Oct. 8, 2012 | 2 a.m.
In a sterile hospital room, 79-year-old Vincent Tortella lies in bed, his eyes blinking and his chest heaving.
"It's hard for me to breathe," Tortella tells a nurse wearing red scrubs. "I can't … can't catch my breath."
Tortella's eyes begin to droop and his words become incoherent. A nearby oxygen and blood-pressure monitor starts flashing red.
"Are you OK, Vinnie?" the nurse asks, nudging Tortella's limp body.
"O2 sat is down to 86," another nurse says. "I'm calling for a crash cart."
A doctor rushes into the room. He checks for a pulse. There is none.
"Call a code 99," the doctor yells, warning staff of a medical emergency requiring resuscitation. "Start chest compressions!"
The scene looks like it could be playing out at the nearby University Medical Center, but it's not.
Welcome to the Clinical Simulation Center of Las Vegas, where hundreds of local nursing students and clinical residents train for medical emergencies by running simulated scenarios with robotic mannequins.
You see, Tortella is a "SIM man," composed of colorful tubes and wires, springs and batteries, and yellow foam surrounded by pink rubbery skin. But just like any human patient, "SIM man" can blink and breathe, bleed and sweat, even pee and poop.
"They're very realistic," said UNLV nursing student Claire Studebaker, 23. "The fact that they talk to you is really cool."
•••
Coolness aside, these mannequins serve an important role in meeting the growing medical demands of the Las Vegas Valley.
Born three years ago out of a necessity for more nurses in Southern Nevada, the SIM Center has become renowned around the world for its cutting-edge way of training physicians and nurses. The SIM Center is now one of the largest centers of its kind west of the Mississippi River, operations director Jackie Kinsey said.
Before these realistic mannequins were created, medical and nursing students poked oranges and even one another to practice drawing blood or inserting intravenous drips into patients. Now, students are able to use mannequins that don't feel pain and can "die" and be rebooted again and again.
"The great thing about mannequins is some of these situations, (students) won't see in their clinical rotations (at UMC), but they can actually practice it on these mannequins," Kinsey said. "The biggest thing they get out of this is patient safety."
With as many as 98,000 people dying each year across the county because of preventable medical errors, the need for medical and nursing students to practice their craft is great, said UNLV nursing instructor Jessica Doolen.
These simulations help students quickly solve medical mysteries on their feet and helps develop their critical reasoning skills, Doolen said.
Unlike a dry lecture on anatomy and physiology, here students can apply their knowledge in simulation and retain the information better, she added. And if students botch the medical procedure, it's on a mannequin — not a human.
"The better students are prepared with simulations, the better prepared they are in hospitals and the real world," Doolen said. "The better prepared they are … we have a healthier community."
However, too often, nursing students and medical residents are educated and trained in silos with little interaction between them. In the real world, such as a hospital or nursing home, doctors and nurses have to learn how to communicate effectively to solve problems, Doolen said.
Often, new nurses can be intimidated by physicians in a hospital, SIM technician Suzanne Sharp said. That makes it difficult for nurses to speak up when they disagree with a diagnosis or raise a concern about a medical procedure that could result in a medical error.
"(Often) when (new nurses) hit the hospital floor, they've never talked to doctors before," Sharp said. "These simulations bring them together. They learn that they have to work together to save a patient."
Nursing students seem to like the SIM labs, calling it a valuable learning experience. However, they contend these stressful simulations can be nerve-wracking at times.
"I'm really shy, so this helps," said UNLV nursing student Amber Anderson, 22. "We learn to get more assertive."
Her classmate Almass Rafi, 26, agreed.
"It's a safe place to make your mistakes," she said. "It lets us make the mistakes before we get to a real-life situation."
•••
Back in the mock emergency room, the "doctor" — a UNSOM medical resident — and eight "nurses" — second-semester UNLV nursing students — are fighting to revive Tortella, a $65,000 "SIM man" who is suffering from a respiratory and cardiac arrest.
As the resident oversees Tortella's vital signs, a nursing student is busy administering chest compressions at a rate of 100 per minute. Meanwhile, "SIM man" is transmitting data to a control room behind the emergency room.
Throughout the simulation, Doolen, a UNSOM physician and a SIM technician are observing the exercise through a one-way mirrored window and two video monitors. The SIM technician, who previously was speaking for Tortella through a microphone and speaker system, now is monitoring the compression rate and depth for the nursing student administering CPR.
Every few minutes, the nursing students are supposed to switch off doing cardiopulmonary resuscitation, but in the heat of the moment, they seem to have forgotten. The compression rate speeds up and slows erratically.
The technician types a note to remind students of this error on the computer. Although these 20-minute exercises aren't graded, they're recorded and reviewed during a 30-minute debriefing session afterward to help students learn from their mistakes.
"Patient is intubated," a nursing student tells the resident inside the emergency room. She places a breathing apparatus over Tortella's mouth.
"Good, continue CPR," the medical resident replies. "We can give 1 milligram of epinephrine."
Another nursing student rushes over to deliver a "demo dose" of fake medication. Everyone has a serious look about them; the simulation has taken on a real life-or-death scenario.
No one has suggested delivering an electric shock using the defibrillator, Doolen notes.
"Let's give them five more minutes," she says.
•••
The 31,000-square-foot SIM Center, at UNLV's Shadow Lane campus near UMC, was the brainchild of UNLV dean of nursing Carolyn Yucha, who came up with the idea during a taxi ride with her counterpart from Nevada State College.
The university and college each had a simulation room, where large, wired mannequins were used by the respective nursing students. These "low-fidelity" — or less realistic — mannequins were heavy and often featured singular body parts such as an arm or pelvis to help nurses practice inserting IVs and catheters.
The new SIM Center was a unique collaborative effort, pooling the two school's resources — as well as those from the University of Nevada School of Medicine — to create a comprehensive simulation center for local nursing students. (The College of Southern Nevada also a simulation laboratory for its students.)
"Getting all the schools together was challenging to get past," Kinsey said. "They all had different visions and curriculum, but they seem to be working well together now."
The SIM Center opened in September 2009, funded with nearly $18 million in state and federal grant funding earmarked by Sen. Harry Reid, D-Nev. Three years later, the center's $566,500 annual operating budget comes from the nursing schools at UNLV and NSC, as well as the state medical school.
Even though it is staffed by just five people, the SIM center, like most medical and nursing schools, is expensive to run.
Some of those costs fall on students. Nursing students pay upwards of $1,500 to use the SIM Center. Medical residents, because they serve their residencies at UMC, can use the facilities for free (their cost is paid for by UNSOM).
There are five laboratories at the SIM Center: emergency rooms, hospital beds, a pediatric room and a delivery room.
The center has nine "high-fidelity," or human-like, mannequins with interchangeable body parts, wigs and mustaches to simulate male and female patients of varying ages.
Jello-like special effects can be added on to simulate gang tattoos and gunshot wounds, various infections, burn injuries and bedsores. Sprays are used to mimic foul odors coming from vomit, excrement and infected wounds to simulate a real hospital scenario.
"You try to make it as real as possible," Sharp said. "You want (students) to suspend disbelief, and they really do."
Smaller mannequins representing a crying infant and 1-year-old and 5-year-old children help pediatric nurses-in-training. In another room, a "SIM mother" can deliver a small "robo-baby" using a mechanic pump in a minute to an hour to simulate childbirth for obstetricians-in-training.
More than 100 simulations can be programmed on the SIM Center's computers and mannequins. Some help students diagnose pneumonia. Others help them save a patient's life.
Higher education leaders hope these lessons will keep generating more doctors and nurses in Las Vegas, which has long suffered a shortage of both. With a new Veterans Affairs hospital that opened in North Las Vegas and plans for a new hospital and senior health care center at Union Village in Henderson, there are burgeoning opportunities in Las Vegas' medical sector.
"This is a whole different kind of learning," Kinsey said. "This center is playing a huge role in trying to make Southern Nevada into a medical mecca."
•••
Doolen paces about inside the control room, waiting for the medical team inside the mock emergency room to administer the correct solution that would save Tortella's life: an electric shock from a defibrillator.
A male nursing student has taken over the compressions and the SIM technician notes his rhythm is more accurate.
The medical resident orders a nitroglycerine patch, then more epinephrine to revive his patient. After a couple of minutes, he calls for the electric shock treatment.
A nursing student places two electrodes on Tortella's plastic-and-latex chest.
"Prepare for shock," he says. "Everyone clear?"
Two fake high-voltage shocks are administered. The medical resident checks for a heartbeat.
"OK, we got a pulse."
A technician's voice suddenly booms over the loudspeakers.
"This simulation is over. Please head to the debriefing room."
CORRECTION: The medical residents are from the University of Nevada School of Medicine, not University Medical Center. The medical residents rotate at UMC, which is UNSOM's primary teaching hospital, but UNSOM sponsors their training and pays their salaries. | (October 8, 2012)

Join the Discussion:
Check this out for a full explanation of our conversion to the LiveFyre commenting system and instructions on how to sign up for an account.
Full comments policy