
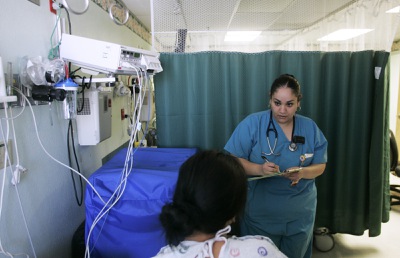
Medical resident Ryan Young performs an amniocentesis at University Medical Center under the guidance of Dr. Marsha Matsunaga Kirgan, left, an assistant professor of obstetrics and gynecology, as resident Evelen Soliman watches.
Friday, April 10, 2009 | 2 a.m.
Sun Archives
- A black eye in medicine brings posturing, again (4-9-09)
- J-1 doctors at UMC: It could benefit both (4-9-09)
- UMC CEO: Bill to open cancer center doesn’t address funding (4-8-09)
- Bill to open UMC cancer center OK’d on party lines (4-7-09)
- Health sciences center in abstract no more (3-11-2009)
- Nursing students to pay for new lab (12-18-2008)
- In infancy, health sciences stumbling (8-11-2008)
- Nevada's goal for health sciences: Unity (1-26-2007)
Sun coverage
Beyond the Sun
Budget reductions are cutting into University of Nevada School of Medicine resident physicians’ training and benefits.
Faced with declining funding, the county-run University Medical Center has closed or is in the process of closing units where the medical residents get hands-on clinical experience including a high-risk obstetrics unit, the University Women’s Center and an outpatient oncology clinic.
Separate cutbacks at the School of Medicine, part of Nevada’s public higher education system, mean some departments are spending less to send residents to conferences where they present the results of medical research and network with colleagues from other institutions.
Residents are new doctors who train under the supervision of more experienced colleagues following graduation from medical school. Physicians tend to stay and practice in states where they complete their residencies, and Peter Brokish, a resident in emergency medicine, told the higher education system’s Board of Regents in February that the financial crisis was affecting recruitment of residents.
“We’re trying to get the best and brightest applicants from other different universities, other medical schools,” Brokish said at the time. “With all the interviews that we’ve done so far, a lot of people are very concerned about the instability that we’re seeing, with all the different changes that are occurring right now. One applicant actually said, ‘It doesn’t look like there’s a lot of stock or priority placed on resident education. What do you think about that?’ And I unfortunately had no answer for him.”
The School of Medicine has more than 260 residents working in fields ranging from family medicine to surgery. Of those, 182 are based in Las Vegas and rotate at UMC for most or part of their training. The effect of budget cuts on education varies by specialty.
Paul Stumpf, chairman of the School of Medicine’s obstetrics and gynecology department, said his residents receive much of their training at the high-risk unit, which UMC shut down in December, and women’s center, which is scheduled to close in May.
Stumpf said to compensate for the loss of the women’s center, residents are transferring to the School of Medicine’s Patient Care Center, which offers comparable services including annual gynecological exams, breast exams and prenatal care.
Residents will see high-risk patients such as those with diabetes or high blood pressure during rounds in UMC’s general obstetrics ward, where those patients are now mixed in with other pregnant women. But as Stumpf said, the closure of the high-risk unit is still a blow.
“It’s a different experience for the resident to be seeing only (the high-risk) patients,” Stumpf said. “It makes the teaching experience at the bedside much more intensive.”
This latest fallout from the financial crisis “puts the community of Las Vegas at risk because UMC is one of the primary institutions that has residency educational training programs,” said Elissa Palmer, chairwoman of the School of Medicine’s family medicine department in Las Vegas.
Residents in her area provide prenatal care at the women’s center, and Palmer said her department is still looking for alternative sites in the valley where residents could offer those services to patients. With UMC winding down the women’s center, residents are seeing fewer patients, said Kate Martin, one of the chief residents in family medicine.
Internal medicine residents who worked in UMC’s outpatient oncology unit, which is no longer accepting new patients, will now train at the Nevada Cancer Institute to get experience in areas such as administering outpatient chemotherapy.
Miriam Bar-on, the School of Medicine’s associate dean for graduate medical education, emphasized that residents will continue getting all the training that the Accreditation Council on Graduate Medical Education requires of approved programs.
Still, despite administrators’ efforts to maintain the quality of programs, residents have seen some benefits erode.
The School of Medicine sometimes pays for the new doctors to attend conferences, covering expenses such as airfares, hotel stays and registration fees. Stumpf’s department managed to preserve these benefits by making other sacrifices, such as trimming some of the same perks for faculty members.
“We’re trying to protect our most vulnerable colleagues, our medical residents and students, and carry that burden on our own backs,” Stumpf said.
Still, other School of Medicine departments have reduced these allowances for residents.
At the February Board of Regents meeting, two medical residents complained that they felt they were getting little support from high-level administrators.
Bar-on said, however, that she has been working to address concerns. Negotiations with UMC regarding food for residents is a case in point.
In the past, residents got to eat free in the hospital cafeteria. UMC absorbed the costs of those meals. Late last year, Bar-on said, UMC surprised her and the residents by announcing that the food would no longer be free. Instead, residents were to get the employee discount.
Bar-on said she worked with UMC officials to craft a compromise. Now, Bar-on said, teams of residents get a debit card that UMC recharges with money to cover meals at the hospital cafeteria while they are on call.
UMC expects to save about $500,000 a year as a result of the change.
“Previously, there wasn’t a limit on the amount of food residents could take from the cafeteria, and the system was being taken advantage of at the expense of UMC and, ultimately, the taxpayers,” UMC spokesman Rick Plummer wrote in an e-mail. He wouldn’t elaborate.
The new food policy “puts us in line with other teaching hospitals around the nation,” Plummer noted.
Steps administrators at UMC and the School of Medicine have taken in recent months should improve communication between the two institutions regarding residency programs.
This year, Bar-on said, UMC’s chief operating officer began meeting regularly with her and attending monthly forums with residents.
Sun reporter Joe Schoenmann contributed to this story.

Join the Discussion:
Check this out for a full explanation of our conversion to the LiveFyre commenting system and instructions on how to sign up for an account.
Full comments policy