
Mona Shield Payne / Special to the Sun
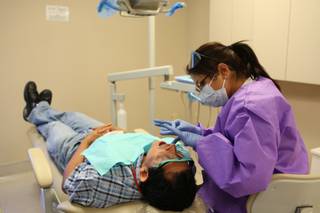
Horencia Sanchez, 36, discusses her dental options Tuesday with office clerk Carmen Garcia at the Nevada Health Centers location at 2212 S. Eastern Avenue. The increase of uninsured patients has hurt the nonprofit Nevada Health Centers, which has 33 locations across the state.
Wednesday, April 21, 2010 | 2 a.m.
Sun archives
Beyond the Sun
The weight of the recession is pushing Nevada Health Centers, the medical safety net for tens of thousands of low-income Nevadans, to the financial breaking point, officials with the nonprofit organization say.
The number of patient visits is up 25 percent to about 205,000 a year, and an increasing number of them — almost three in 10 — are uninsured, Nevada Health Centers CEO Tom Chase said. And when the uninsured agree to greatly reduced payment plans, they frequently stiff the agency.
The result is what Chase diplomatically calls a “cash pinch.” The organization is behind in paying its own bills, has had to restrict access for patients who don’t pay their bills and came close to not meeting payroll, he said.
This month the federal government gave Nevada Health Centers temporary reprieve in the form of a $1.7 million advance on a $35 million, five-year grant. Now the organization has about $750,000 in the bank, with expectations that it will increase, Chase said.
Chase is scheduled today to talk about his organization’s struggles before the Legislative Committee on Health Care. Over the long haul, if the recession continues, services to people who can’t pay will be limited unless the payer mix can be improved, Chase said.
“We’re going to be forced to make hard decisions about services and sites,” he said.
More than 600,000 Nevadans are expected to be without health insurance in 2010. Nevada Health Centers is a $28 million organization that qualifies for federal grants and funding because its 33 locations are in far-flung towns such as Beatty and Elko and blighted urban parts of Las Vegas and North Las Vegas. Patients who qualify get discounts on services. A typical physical examination and medical history, with lab tests, costs about $45 for a low-income patient — about half what it costs the organization, Chase said.
The organization’s struggles are bad news for people such as Patricia Annis of Henderson. Annis, 67, is a retired legislative aid whose teeth are breaking. She’s desperate for care and heard about a Nevada Health Centers’ program providing free dental work to low-income elderly patients. Her $733 a month in Social Security income qualifies her.
“I’ve had two teeth die on me,” Annis said. “I’ve had to find a way to get temporary treatment from a private dentist, but I need a root canal.”
The problem is Nevada Health Centers is flooded with low-income elderly with dental needs, Chase said. The $150,000 dental-care grant was divided evenly between Nevada Health Centers in Elko and Las Vegas, and the money is going fast, Chase said.
“The need is incredible with each of these patients,” he said. “They’ve had no dental work in years.”
Annis has been on the waiting list for months and is frustrated with Nevada Health Centers. But Chase said it’s slow going because his people are doling out the grant funds patient by patient, sometimes as much as $4,000 a pop.
Chase said the payer-mix problem is partly attributed to the low percentage of patients covered by Medicaid, the state government’s insurance program for low-income residents. Most federally qualified health centers have 36 percent of their patients covered by Medicaid, he said, but it’s only about 20 percent for Nevada Health Centers.
That’s because customers of Health Plan of Nevada, the managed care organization owned by UnitedHealth Group, which is part of the Medicaid program, has a closed network of doctors, so its patients can’t go to Nevada Health Centers, Chase said.
Chase said Medicaid patients are supposed to be allowed to choose a federally qualified health clinic such as Nevada Health Centers.
“All I ask is that (Health Plan of Nevada) patients, who have chosen to enroll in that network, be afforded the opportunity” to come to Nevada Health Centers, Chase said. “We think when they come they’ll like us and they’ll stay. My problem is they’re not even allowed to come.”
Chase said he has spoken with Health Plan of Nevada officials and they agreed to examine their allocation of Medicaid patients.
“I expect we will see a more robust Medicaid mix,” he said. “It’s taken getting to this stage for everybody to realize how important that is.”

Join the Discussion:
Check this out for a full explanation of our conversion to the LiveFyre commenting system and instructions on how to sign up for an account.
Full comments policy