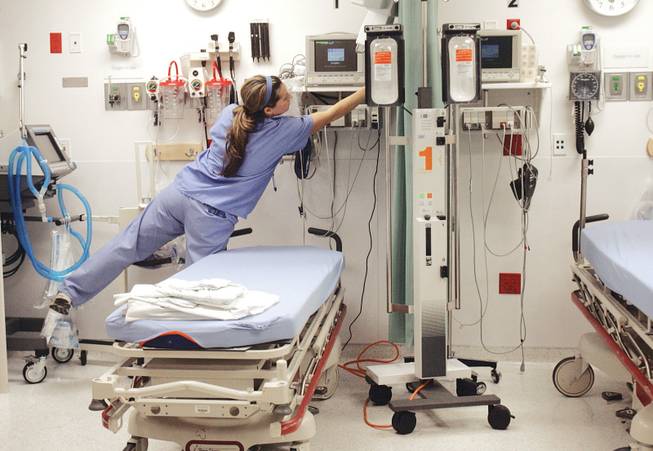
Registered nurse Nicole Evans straightens up a room in the trauma center at St. Rose Dominican Hospital — Siena Campus in 2008.
Friday, May 31, 2013 | 2 a.m.

Brian Brannman
State investigators have found a pattern of improper patient transfers by St. Rose Dominican Hospitals — Siena Campus to the region’s only public hospital, University Medical Center, according to documents obtained by the Las Vegas Sun.
UMC CEO Brian Brannman said the practice could be contributing to financial shortfalls at UMC and is worsening the overcrowding of its emergency room.
“We want to be the community’s hospital, but we need to be a lot more protective of taxpayer dollars and not get run over,” Brannman said after reviewing the documents, obtained by the Sun through a public records request.
Clark County Commissioner Chris Giunchigliani said the investigation confirms long-held suspicions: “The fact that it was systemic and substantiated that they were inappropriate is consistent with what many of us have thought.”
Depending on how common the practice is at St. Rose and other private hospitals, the transfers of patients could be costing UMC — and, thus, county taxpayers — millions of dollars to treat uninsured or underinsured patients. Conversely, hospitals that are sending patients to UMC are saving a like amount of cost on their books.
According to data supplied by UMC, St. Rose Siena transferred 78 patients to UMC between August 2011 and May 2012, more than any other valley hospital.
UMC’s current deficit is about $30 million.
Rod Davis, senior vice president of operations of St. Rose parent company Dignity Health Nevada, released a statement to the Sun saying that St. Rose is a faith-based, nonprofit institution with a mission to serve the indigent. The transfers, he said, were medically necessary — a claim disputed by UMC. Because the patients transferred from St. Rose Siena to UMC in 2012 were more likely to be insured than the typical UMC patient, St. Rose is actually helping UMC, Davis said.
Regardless of the financial outcome, “The findings of this investigation indicate the hospital’s actions and use of internal policies were not in compliance” with state law, according to the documents.
Investigators with the state Department of Health and Human Services reviewed just a sample of patient transfers and found 13 that were “inappropriate.” Investigators give a score based on severity and scope. The St. Rose severity score indicates patients were not put at risk due to the transfers.
The scope score, however, indicates the problem is systemic, meaning it has been a routine practice to move patients from St. Rose to UMC in violation of state and possibly federal law.
The Centers for Medicare and Medicaid Services, the powerful federal health regulator, will likely now determine if St. Rose is operating in compliance with the Emergency Medical Treatment and Active Labor Act, known in the health care industry as EMTALA.
The law requires hospital emergency rooms to provide care or arrange for services with another hospital if it is unable to do so. If its own specialists are not available, the hospital is required to transfer the patient to another hospital that can provide the care. St. Rose has a transfer agreement for these circumstances with UMC.
Marla McDade-Williams, deputy administrator of the state Health Division, said hospitals should have specific, transparent policies communicated to their staff, patients and the receiving hospital — UMC — about when specialists are not available and therefore when patients will likely be transferred. Instead, St. Rose appears to have a looser, more open-ended arrangement of transferring patients without specific guidelines, McDade-Williams said.
In Brannman’s view, this opens the door for abuse.
Of the 13 patients, whose names and attending physicians are redacted, most required a urologist, neurologist or opthalmologist. In each case, St. Rose says a proper specialist was unavailable, requiring the transfer to UMC.
“St. Rose Dominican Hospitals has internally reviewed every patient transfer to UMC, and all were determined to be required for medical necessity,” Davis said in the statement.
UMC officials are skeptical of the claim. Many of the patients supposedly in need of a specialist don’t actually need such treatment and could often be treated by a competent emergency room physician, Brannman said.
In one of the cases reviewed by investigators, for instance, a patient went to St. Rose after he tried to remove his own genital warts. He was sent from St. Rose to UMC, ostensibly to see a urologist. At UMC, however, his wound was sutured and he was discharged without the need for a specialist, an outcome that just as easily could have been achieved at St. Rose, Brannman said.
In another case, a patient suffered a stroke, fell and bumped his head. He was transferred to UMC, much to the chagrin of the neurologist there, who said he could have been treated at St. Rose, which markets its own stroke treatment program.
UMC also suspects specialists would become available at St. Rose if the patient were deemed financially desirable — meaning well-insured.
“If it’s the right patient at the right time, they’re able to find the (ear, nose and throat) doctor. But the other patients — they don’t want to be bothered,” Brannman said.
Brannman said the practice of moving undesirable patients is not unique to the Las Vegas market, but said UMC faces greater challenges because of its status as the region’s only public hospital.
“We’re it. We’re the only one. So there’s a real incentive for them to use us to streamline their patient mix,” he said, meaning save the best-insured patients for themselves while sending the others to UMC.
“The reason these private hospitals can be so profitable is because we’re here to take the losses,” Brannman said.
Davis noted in his statement that the proportion of patients transferred to UMC from St. Rose who have insurance is 19 percentage points higher than the typical UMC patient mix. Meanwhile, the percentage who have no insurance or rely on Medicaid — 26 percent — is much lower than usual for UMC.
Based on that data, Davis said, “These medically necessary transfers have actually benefited UMC’s payer mix and financial health.”
Brannman responds that the data come from St. Rose Siena, which is in one of the most affluent areas of the city. He said he suspects data from St. Rose's Rose de Lima Campus, which is located on the more working-class Lake Mead Parkway, would show a different result. The Las Vegas Valley’s three St. Rose Dominican Hospitals transferred a total of 186 patients to UMC between August 2011 and May 2012; 38 percent were Medicaid or uninsured patients — generally considered financially undesirable.
Also, not all insurance is created equal. Some health management organizations reimburse at less than cost; just because a patient is insured, doesn’t mean he’s financially desirable, Brannman said.
Finally, Brannman said, although the payer mix may be an improvement for UMC, it’s still not a healthy payer mix — it’s just less bad.
Brannman said patient transfer agreements like the one with St. Rose are not unusual but should not be viewed as a substitute for good clinical decision-making. “The spirit is that we make ourselves available for services other hospitals don’t have. But it can serve as gateway to get dumped on. It creates an avenue for abuse.”
Even if St. Rose determines it doesn’t have a specialist available, it is obligated to bring patients to the closest hospital that does, which would usually be Sunrise Hospital & Medical Center, Brannman said. But in each case flagged by state investigators, the patient was transferred to UMC rather than Sunrise.
Brannman said the patient transfers clog an already sclerotic UMC emergency room.
By clearing out patients, St. Rose can market shorter ER wait times while also opening up beds for lucrative elective surgeries.
Brannman said frequent transfers are not consistent with high-quality care: “If a patient has something beyond their capability, they should be transferred. But if not, the patient is being moved around and inconvenienced and incurring additional cost, and that’s not good patient care. Are we doing right by the people who come to us expecting to be taken care of?”
Brannman said he hopes the state investigation is just the beginning of a process that will bring needed relief to UMC.
“It’s worth getting aggressive and looking at this. Las Vegas has been the Wild West in health care for a long time. Hopefully we’ll get out of the old way of doing things and start being more professional,” he said.
St. Rose transfer policies are already under scrutiny stemming from lawsuits of two doctors who allege they were fired when they refused to transfer patients because they felt it would threaten patient safety. In those cases, the doctors allege they were encouraged — with cash bonuses and the threat of discipline — to shuttle patients from St. Rose Siena, the company’s busiest, to the less crowded San Martin campus in the southwest valley. This would open up beds at Siena for financially advantageous elective surgeries, the doctors allege.
St. Rose has said its aggressive transfer policy between its hospital campuses is meant to relieve overcrowding. The hospital also says in the lawsuits that it can’t be held responsible for the actions of emergency room management because it employs a contractor, Emergency Medicine Physicians, to run its emergency department. Shortly after a Sun story about the lawsuits, St. Rose terminated its relationship with Emergency Medicine Physicians.
Emergency Medicine Physicians remains the ER contractor, however, at UMC.


Join the Discussion:
Check this out for a full explanation of our conversion to the LiveFyre commenting system and instructions on how to sign up for an account.
Full comments policy