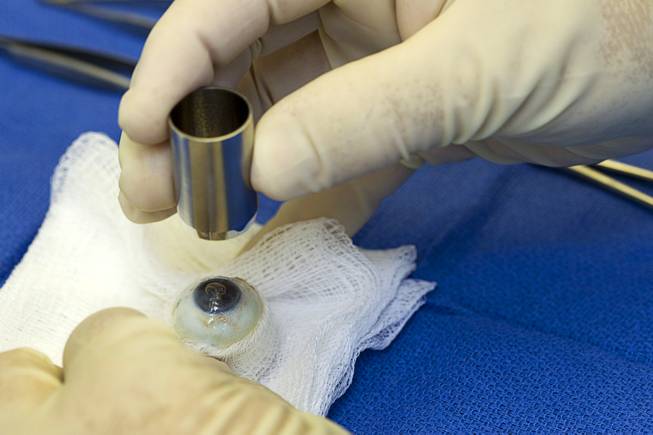
Brent Bergquist, director of ocular services at the Nevada Donor Network, holds a trephine, a surgical instrument with a cylindrical blade, at the Network offices Tuesday, July 22, 2014.
Sunday, July 27, 2014 | 2 a.m.
Related story
For Brent Bergquist, staring at the faces of the dead is part of his job.
“I’m looking at their eyes and looking at their facial expressions ... I wonder what they’re like. Were they sad? Were they happy? Did they go peacefully?”
For Bergquist, this moment is as intimate as it gets. In the few seconds before the corneal procurement begins, he tries to see these people for who they were and how they lived.
He pushes a cylindrical saw into an open eye and twists, cutting the tough surface. He removes the cornea, the first clear layer before the colored iris.
At 47, Bergquist is a veteran corneal procurement technician who views the procedure as a ritual in altruism. He knows the corneas he removes will be used to restore someone’s sight.
Lighthearted and garrulous, Bergquist likes to talk about his work. He has an obvious passion for it.
“I would venture to say that I feel like I’m doing something for them,” he said. “I’m completing their wishes.”
The sight of more than a million men, women and children has been restored through corneal transplants since 1961, according to the Eye Bank Association of America, the world’s leading organization on cornea transplants. Donations are so effective that it is the only transplant for which there is no waiting list. That’s largely because corneas are avascular, meaning they don’t have blood, making them universally matchable.
Bergquist has done the procedure hundreds of times. Now director of ocular services at the Nevada Donor Network, he is undaunted by the cold, blank face of death.
Bergquist’s workroom smells like disinfectant and hand sanitizer. There’s not a paperclip out of place. The corneas are stored in transparent plastic cases filled with a clear preservative liquid.
Bergquist always wanted a career in the medical field. He started college at UNLV to be a physical therapist, like his father. One of his first jobs, at 18, was as a University Medical Center transporter.
Corneal procurement is not for queasy stomachs or superstitious hearts.
“Some people, they think they can do it, but then they look into the eyes, and they realize they can’t,” Bergquist said.
First, technicians examine the body, checking for growths, sores, signs of disease. They have to know the donors, their social and medical backgrounds. Bergquist knows names, ages and causes of death.
For him, death always has been a candid topic.
“Death is not a big deal,” he said. “It’s just another step … I’ve never been creeped out by it.”
His outlook is due largely to his faith. A devout member of the Church of Jesus Christ of Latter-day Saints, it is Bergquist’s certainty of a blessed afterlife that calms him in morgues and funeral homes.
“For some people, it’s so final, it’s so terrible,” he said. “I don’t know how they do it.”
Bergquist’s first retrieval, he admits, was a learning experience. But he is devoted to giving back, and this line of work allows him to do that in a significant way.
“I prayed the first time, and I’ve prayed ever since,” he said. “I did have a certain amount of reverence for that person. To me, it’s such a sacred thing for them to donate.”
The truth behind organ harvesting
We’ve all seen it: that box on driver licenses and state ID applications that asks whether you’d like to be an organ donor.
While the idea of having your body divvied up after death is off-putting to some, for the more than 114,000 Nevadans in need of an organ transplant, that check means a chance to live. A single organ donor can save up to eight lives and heal more than 50 people.
The transplant process is run by specialized professionals designated to navigate the emotions and logistics involved.
Before harvesting begins, several tests are done to confirm that someone really is dead and beyond saving. If you’ve indicated that you want to be an organ donor, someone designated with power of attorney must sign a consent form before the process can begin. If a patient’s wishes are unclear, hospital staff will discuss options with family members, who have the final say.
Some people worry doctors might not try as hard to save your life if you’re an organ donor. Not true. Transplant teams don’t get involved until a separate team of physicians has determined that death has occurred.
The organ removal process is performed in an operating room, and patients are sewn up so their body still can be visited and viewed.
Surgical specialists conduct the procedure, but transplant coordinators walk loved ones through the process.


Join the Discussion:
Check this out for a full explanation of our conversion to the LiveFyre commenting system and instructions on how to sign up for an account.
Full comments policy