
Shutterstock.com
Since 2013, when changes in Nevada law took effect, it has been among the best states for aspiring parents who want or need to use assisted reproductive technology.
Monday, Feb. 13, 2017 | 2 a.m.
Hundreds of thousands of women around the world give birth daily, more than 10,000 here in the U.S. alone. Yet having a baby does not come easily, or even naturally, for some.
Around 7.5 million American women ages 15 to 44 — more than 12 percent — have difficulty either getting pregnant or carrying a baby to term, according to the Centers for Disease Control and Prevention (CDC). And while age remains the greatest factor affecting fertility, almost half of those signing up for reproductive assistance are younger than 35.
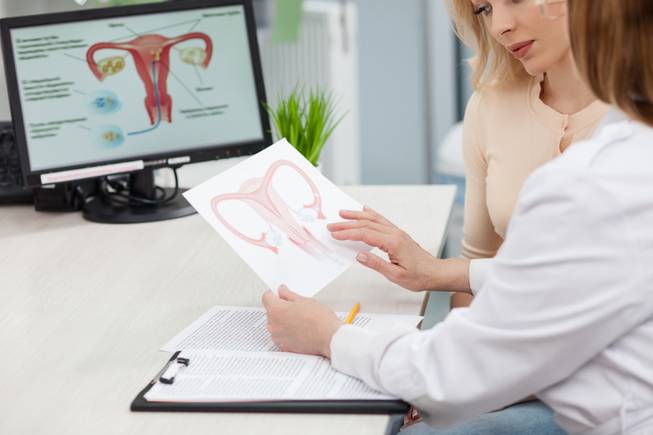
Brianne Luckman is part of that statistic. After trying from the age of 23 to get pregnant, she knew after a year that something was wrong. Numerous tests and a string of diagnoses made her desire to be a mom seem like a pipe dream. First a thyroid problem caused her to miscarry.
“I managed to even out my thyroid, but then I found out I had polycystic ovary syndrome,” Luckman said.
By the numbers:
• 11.3% (almost 7 million): Women ages 15 to 44 who have used infertility services
• 1 million to 2 million: The number of eggs the average woman is born with
• 25,000: The number of eggs the average 37-year-old woman has left
The hormonal disorder causes irregular periods and enlarged ovaries with small cysts, and complications include eggs not developing or being released normally. After having it treated and still failing to get pregnant, Luckman sought further tests that revealed her husband, Will, was afflicted by low sperm motility.
“I started to wonder: What is going on with me?” Luckman said. “I always felt like I was born to be a mom, and with all of these setbacks, I believed I would have to face my biggest fear: that this wasn’t going to happen for us. That was a really difficult reality to face.”
When the decline in egg reserves and quality tied to “advanced maternal age” (older than 35) isn’t the culprit, the multifactorial nature of infertility is underlined. “It’s so hard to put a finger on it and just blame it all on the eggs. Forty percent of infertility is related to the woman, 40 percent is related to the man,” said Dr. John V. Martin, a private-practice OB-GYN with Women’s Health Associates of Southern Nevada who has served the Las Vegas Valley for more than two decades. The other 20 percent of infertility cases, he said, can be the most vexing because they’re “unexplained.”
From 2003 to 2013, use of in vitro fertilization (IVF) in the U.S. increased 65 percent, which seems to suggest infertility is on the rise. But Dr. Bruce Shapiro, founder of the Fertility Center of Las Vegas and director of the University of Nevada School of Medicine’s Division of Reproductive Endocrinology and Infertility, said it’s not that more women are having fertility issues. More are getting tested.
“Younger women who are in a position to want to have children are choosing to try to do so earlier to avoid problems that might be associated with a delay in childbearing. So they are finding out about reproductive challenges sooner,” he said. “Then we have another group of women who know for certain that they don’t want to become pregnant right now, so they undergo the required fertility tests prior to cryopreserving, or freezing their eggs.”
Shapiro said early testing and advances in technology mean more couples can combat infertility. IVF success rates are much higher than they were 30 years ago. But CDC data show that even if you get pregnant through IVF, that doesn’t always result in a baby. “For example, 93,787 fresh nondonor ART cycles were started in 2013. Of those, 33,425 (36 percent) led to a pregnancy, but only 27,406 (29 percent) resulted in a live birth. In other words, 6,019 (almost 1 in 5) of ART pregnancies did not result in a live birth,” reads a 2013 report on success rates provided by 467 fertility clinics in the U.S. On the flipside, the increased efficiency of the procedure, whereby eggs are fertilized outside of the body, can be cost-saving, Shapiro said. “Some people, from one (egg) retrieval cycle, can now have their entire family, one baby at a time.”
Costing more than $30,000, IVF is generally described as expensive, frustrating and intensely emotional. But when it’s successful, the same five words seem to be echoed by new parents: It was all worth it.
• • •
Four months after completing the required tests, Luckman commenced egg harvesting for IVF. She produced 21 eggs, but only five “took,” and only two made it to the embryo stage.
“I was very disappointed that so few eggs made it. And then when I started the egg transfer, it was a whirlwind of emotions, just hormones and injections,” she said, adding that the process doesn’t favor shyness. “You basically feel like you have your pants off all the time, and the faster you get used to it, the less anxiety you’ll have.”

Will and Brianne Luckman with baby Owen.
From passing out and falling on her face while injecting hormones to piling up expenses and then debts that created tension in her marriage, Luckman describes a nightmarish road to having her dream of a family. But she did conceive, and after surpassing the 12-week danger zone, memories of the emotional roller coaster and feeling of being a human pincushion all slipped away.
“You begin to create a bond with this miracle, this life growing inside of you,” she said of baby Owen, who turned 1 at the end of January. “For me, as a woman, not to have been able to experience that, I probably would have been devastated.”
The Luckmans will go through IVF again in June, and their doctors believe they’ll have success, in great part because they caught their problems early.
“Between 35 and 36, people generally do OK,” said Dr. Carrie Bedient, a reproductive endocrinologist and fertility specialist at the Fertility Center of Las Vegas. “But 37 through 39 is where I see the biggest drop in success rates.”
Trina Morella achieved success with IVF eight years ago, but now, at 42, with no eggs stored and poor reserves, her chances of having another child that is biologically hers are slim. She could find an egg donor, or adopt an embryo leftover from another couple’s IVF cycle. Failing that, she could call on a surrogate.
“We think about growing our family often, but I don’t know that I necessarily need to be pregnant in order to do that again,” said Morella, adding that she is considering adoption. “My husband and I are still discussing how we’re going to achieve that.”
Women are born with a finite number of eggs and have a steady rate of attrition throughout their reproductive years. While fertility factors are very individualized, it’s generally accepted that by age 40, a significant number of women — some studies suggest it’s as high as 50 percent — have difficulty conceiving with their own eggs.
Harvesting and freezing eggs at a younger age, while reserves are still high, can enable older women to get pregnant through IVF using embryos at lower risk for chromosomal abnormalities, though they may contend with complications. Martin listed higher incidences of gestational diabetes and preeclampsia (a potentially dangerous condition characterized by high blood pressure) in women of advanced maternal age, but emphasized that the chance is probably less than 15 percent. He also said that reproductive technology has “improved immensely” while he has been in practice.
“I think that women just have to be aware of what’s available. The biggest thing that I find myself doing more than anything, is reassuring women that they still can try to have a baby. Where I start to put pressure on them is when they’re 40 or older. I say, ‘You know, this is really time. You have to decide, and you have to do some soul searching — What do you want?’” Martin said. “(IVF) is a huge sacrifice. It’s a financial sacrifice; it’s a personal sacrifice; it’s a physical sacrifice. And these women are just so dedicated to trying to have a child or another child, that nothing will deter them. … It’s a special thing — you can never lose sight of what a significant event the birth of a child is.”
-

FACTORS THAT CAN AFFECT FERTILITY
The psychological impact of infertility
“While the causes of infertility are overwhelmingly physiological, the resulting heartache — often exacerbated by the physical and emotional rigors of infertility treatment — may exact a huge psychological toll,” reads a Harvard Medical School mental health bulletin. Half of women find the process to be the most upsetting experience of their lives, and infertility has been shown to leave sufferers as anxious or depressed as those diagnosed with cancer. Hormone treatments can have emotional side effects. Money worries can overwhelm. And feelings of disappointment and inadequacy can deepen profoundly if treatments ultimately don’t work. “It’s also difficult to know when to stop seeking treatment. Frequently one partner wants to end treatment before another, which can strain the relationship. Most patients need to gradually, and with great difficulty, make the transition from wanting biological children to accepting that they will have to pursue adoption or come to terms with being childless.”
Unexplained infertility
If all available testing yields nothing that should hinder a couple’s ability to conceive, they are diagnosed with “unexplained infertility.” These couples (up to 20 percent of cases, according to Harvard Medical School) may become pregnant without medical interventions, and the odds may significantly increase with minimal treatment.
• Age in women: The greatest factor affecting fertility, as the quality and quantity of eggs decline over time. Women are born with 1 to 2 million immature eggs, or follicles, and begin puberty with about 300,000. But according to the American Society for Reproductive Medicine, only about 300 follicles will be ovulated during the entire span of a woman’s reproductive years. Generally, women are most fertile in their 20s. By their mid- to late-30s, the egg reserve is depleted, and those remaining may suffer from chromosomal abnormalities that can lead to miscarriage or disorders such as Down and Turner syndromes. After age 40, as many as half of women experience difficulty getting pregnant.
• Age in men: The quality of sperm deteriorates somewhat as men age, but it generally doesn’t affect fertility before they reach their 60s. In the years beyond, there is a slightly higher risk of gene defects, but there is no maximum age for men hoping to father children. Typical causes of male infertility are low sperm count and low sperm quality, though lifestyle choices and medical conditions can have an effect.
• Endometriosis: This affects 176 million globally and 1 in 10 women and girls in the U.S. The disorder, in which the tissue that lines the uterus grows outside of it, can result in damage to the ovaries and more rapid reduction of the egg reserve. Symptoms usually occur between age 12 and 60, and may include abdominal and back pain during menstruation, as well as severe cramps, abnormal or heavy bleeding during periods, painful sex and difficulty getting pregnant.
• Alcohol and tobacco: Heavy drinking has been linked to lower sperm counts, erectile dysfunction and an increased risk of ovulation disorders. The Mayo Clinic suggests avoiding alcohol completely if you are trying to get pregnant. Tobacco smoke is toxic and prematurely ages the ovaries and depletes the eggs. Smoking also can damage the DNA in sperm, which can lead to infertility or problems during pregnancy.
• Cancer treatment: Chemotherapy and radiation speed the depletion of the egg reserve.
• Timing: Infertility may come down to something as simple as timing. Even the most fertile couple will have, at best, a 25 percent chance of conceiving in any given month with perfectly timed intercourse. The fertile window is open four to five days prior to and during ovulation, and it is recommended that you have sex every 24 to 48 hours during this period.
• Medications: Some drugs are not safe for women trying to conceive. And steroids, testosterone replacements and prescription medication may retard or halt sperm production in men. Have an open conversation with your partner and your doctor about all medications and supplements you are taking before trying to conceive.
• Obesity: For women, the Cleveland Clinic lists hormonal changes that lower the chance of natural or technology-assisted conception, and insulin resistance that can disrupt regular menstruation and egg production. For men, it’s a drop in testosterone and a higher rate of erectile dysfunction.
• Vigorous physical activity: Maintaining a healthy lifestyle and weight can be beneficial to fertility, but exercising too hard may inhibit ovulation and reduce the production of the hormone progesterone, which helps to prepare the lining of the uterus to receive a fertilized egg.
-
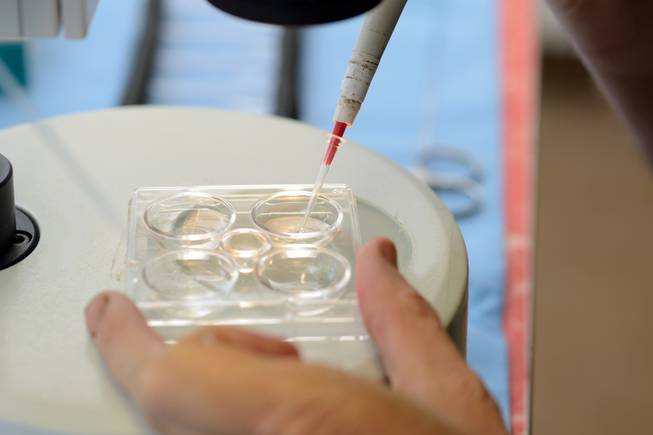
COMMON APPROACHES TO INFERTILITY
If you are having trouble conceiving, it’s important to know that you are not alone. Infertility affects some 7.5 million American women. But advances in science and technology mean more babies are being born to reproductively challenged couples. In fact, according to the National Institutes of Health, more than half of couples with fertility issues become pregnant after treatment, and that’s not including more advanced procedures such as IVF.
The method your doctor recommends will largely depend on the cause of your infertility. Read as much as you can and ask every question, because there are dozens of avenues. These are the most common methods:
More resources
• American Society for Reproductive Medicine — asrm.org
• Resolve: The National Infertility Association — resolve.org
Fertility drugs
• Best for: This course is recommended to women who have healthy fallopian tubes but don’t ovulate regularly, or who have partners with poor sperm quality. Usually the first choice because of affordability and convenience.
• Process: The drugs are injected or taken in pill form, releasing hormones that induce ovulation to boost egg production and make the uterus more receptive to egg implantation.
• Cost: Varies from under $100 to $6,000, depending on whether pills or injectables are used and whether blood tests and ultrasounds are included.
Donor sperm
• Best for: Couples where the male is infertile or has a genetic disorder that could be passed along to the child (and often used by single women and lesbian couples). Some aspiring parents may not be comfortable with the idea of a child who bears none of the father’s genetics, but it’s a popular option due to the simplicity of the procedure.
• Process: Most couples go through a sperm bank. As an example of how donors are screened, the 40-year-old California Cryobank accepts only 1 percent of applicants, recruiting men ages 19-38 from “top U.S. universities” who are at least 5-foot-9 and in good health (those are the basics just to get in the door to be considered).
• Cost: It runs about $500, and the success rate is high.
Surrogacy
• Best for: Women who are able to achieve pregnancy with their own eggs but are unwilling or unable to carry the baby.
• Process: IVF is used to fertilize the egg, and the embryo is then implanted into the surrogate.
• Cost: Considering fees for a surrogate agency and compensation and care for the gestational surrogate, this option can cost as much as $100,000. Numerous legalities (and the cost of related services) need to be considered.
Donor eggs
• Best for: Women with damaged or prematurely failing ovaries, older women with poor egg quality and those who have undergone chemotherapy or radiation. Donors can be found through an agency or known to the prospective parents. Profiles with photos, personal details and medical history can help couples choose a donor, and face-to-face meetings are an option — as are arrangements that allow for a sustained connection, should the child ever want to know his or her biological mother.
• Process: Eggs are harvested from the ovaries of another woman (usually younger) and fertilized by the sperm of the recipient’s partner. Resulting embryos are implanted into the recipient’s uterus.
• Cost: Including IVF and compensation for the donor, the procedure can cost more than $30,000.
Donor embryos
• Best for: Couples unable to produce a viable embryo through IVF
• Process: Embryos are donated by couples who underwent IVF and don’t need their unused fertilized eggs. These are implanted into the recipient, who will have no biological relation to the child, but will experience pregnancy and birth.
• Cost: It is a complex, expensive procedure (up to $30,000), and donors may be scarce, as some couples don’t like the thought of their biological child in another family. While obtaining legal counsel may increase costs, it should reduce or eliminate the potential for litigation.
Artificial insemination
• Best for: The procedure is favored when men have slow-moving or low-quality sperm, or if women have produced sperm antibodies or their cervical mucus doesn’t aid in transporting the sperm to the egg. It also is commonly employed by lesbian couples.
• Process: Sperm is inserted directly into a woman’s cervix, fallopian tubes or uterus.
• Cost: Less than $1,000.
Reproductive surgery
• Best for: Correcting anatomical abnormalities, removing scarring and clearing blockages in the reproductive systems of men and women. Sometimes a hospital stay is required, but surgery also is done on an outpatient basis.
• Cost: Varies depending on the complexity of the procedure and the operating surgeon. Minimally invasive laparoscopic surgery for endometriosis ranges from $2,000 to $5,000, whereas removing damaged fallopian tubes costs $8,000 to $13,000.
In vitro fertilization (IVF)
• Best for: Couples with unexplained infertility and women who are older, have blocked or severely damaged fallopian tubes, or scarring from endometriosis.
• Process: Harvesting eggs and fertilizing them with sperm in a lab. Once embryos develop, one or more are implanted in the uterus, and the remaining embryos are frozen to be used or discarded at a later date. IVF is physically demanding and invasive
• Cost: Insurance often does not cover the expenses of IVF. And several cycles may be required before pregnancy is achieved, with each costing $12,000 to $15,000, not including medications. And it may not work.
Choosing a treatment center
Fertility clinics report success rates to the CDC. Four local clinics pop up in its database (Nevada Fertility Institute (8285 W. Arby Ave., Suite 275) wasn’t established during the last data collection in 2014), and for each, consumers can view a profile of services, patient characteristics, success rates and detailed data summaries. Visit cdc.gov/art
• Sher Institute for Reproductive Medicine: 5320 S. Rainbow Blvd., Suite 300, haveababy.com
• Green Valley Fertility Partners: 2510 Wigwam Parkway, Suite 201, greenvalleyfertility.com
• Red Rock Fertility Center: 9120 W. Russell Road, Suite 200, redrockfertility.com
• Fertility Center of Las Vegas: 8851 W. Sahara Ave., Suite 100, fertilitycenterlv.com
-
IF YOU’RE THINKING ABOUT GESTATIONAL SURROGACY
Legal considerations
Since 2013, when changes in Nevada law took effect, it has been among a handful of best states for aspiring parents who want or need to use assisted reproductive technology (ART). In fact, the Silver State has found favor with Europeans who travel here to take advantage.
“Las Vegas is not only an amazing travel destination, but the state of Nevada is also home to some of the most friendly and secure reproductive laws in the U.S.,” said Dr. Bruce Shapiro, founder of the Fertility Center of Las Vegas, which has served patients from every state and more than 70 countries.
Some countries restrict the use of ART, says Dr. John V. Martin, a private-practice OB-GYN with Women’s Health Associates of Southern Nevada, noting an increase in medical tourism to take advantage of Nevada’s laws around gestational surrogacy. France, for example, doesn’t allow surrogacy, and until China changed its one-child policy, Martin saw patients using U.S. surrogates as a workaround.
But the practice is still relatively new. Martin’s first surrogate delivery was eight years ago, and he recalled how unprepared the hospital was to deal with the legal dynamics between the woman giving birth and the genetic parents.
Other dynamics apply to situations where intended parents divorce after creating a supply of embryos, or pay to acquire biologic materials from another source.
While obtaining legal counsel may increase costs of ART on the front end, having attorneys represent all involved from the very beginning should reduce or eliminate the litigation nightmares that could otherwise arise.
For those contemplating reproductive assistance, attorney Patrick McDonnell with Marquis Aurbach Coffing offered a primer on legal aspects to keep in mind:
#1 Depending on the type of reproductive assistance you seek, it may be mandatory to acquire legal counsel.
“The most complex laws are around gestational surrogacy,” McDonnell said, “and Nevada law stipulates that those involved must have legal representation at the very start of the process, before the gestational carrier commences taking the necessary medication to prepare her body to carry the child.”
While the agreement should be customized to reflect the desires of each intended parent and surrogate, there is a framework defined by the state that ensures the gestational surrogate gives up all rights to the child. While visitation theoretically could be written in, McDonnell said he would advise strongly against it, as it opens to the door to “myriad potential complications for everyone involved.”
“With the intended parents, before I say what I would advise, I would have to do a long interview with them to understand: What are their religious beliefs? What is their position on abortion? What are their priorities here? Is it their priority that they want to have a child no matter what, or is their priority that they only want to have a child who is 100 percent healthy? Are they willing to have a child no matter what the outcome may be? So it would start with a lot of questions from me to my client, as to what’s most important to them,” McDonnell said.
He explained that the agreement should explicitly cover situations where there is something severely wrong with a fetus, or selective reduction is recommended to ensure the health of the carrier and child in cases where more than one embryo was implanted. Considering all possibilities on the front end protects against legal snarls.
That includes the payment particulars, which can be structured in any way agreeable to the parties. McDonnell would advise a surrogate to require living and medical expenses as well as general compensation. If she has younger children, a nanny might be retained to assist through the last portion of the pregnancy and the time immediately following. She may desire a gym membership to address the physical changes that occur through pregnancy, or counseling to deal with any emotional impacts from the experience (though most surrogates have been through the process with their own kids, and may have been further prepped by an agency).
McDonnell said that most agreements include a provision for a term life insurance policy for the gestational carrier that extends about 10 months from the date of the pregnancy. That ensures the carrier’s family would have “a substantial amount of economic impact protection” in the case of her untimely death. The amount can be increased to include a portion for the intended parents, as they are investing a great deal in their effort to have a child.
“In my opinion, the gestational surrogacy agreement should never only cover the bare minimum requirements of the statute,” McDonnell said, “but exactly what those additional provisions will be are unique to each situation.”
#2 The intended parents can use the same attorney, but the gestational carrier must have independent legal representation.
#3 Two intended parents are not required.
#4 If there are two intended parents, they do not have to be married or in formal domestic partnership, and they do not have to be heterosexual.
#5 The intended parent(s) can pay a gestational carrier and/or donors of sperm, eggs or embryos. This is not allowed in some states, and the ability to pay under Nevada law greatly increases the pool of potential donors and carriers.
#6 The child does not have to have a genetic link to the intended parent(s). However, under Nevada statute, the gestational carrier cannot be the egg donor. “The intended parent(s) must utilize either the egg of an intended mother or an egg donation from another third party,” McDonnell said.
#7 As long as the child is to be born in Nevada, the intended parent(s) or the prospective gestational carrier can commence a proceeding in any Nevada district court to obtain an order designating the content of the birth certificate to list the intended parent(s) as the parent(s) of the child, and this proceeding can be commenced prior to the birth. This can nip many potential complications in the bud. McDonnell suggests utilizing a gestational carrier who lives in Nevada. If this is not the case, he advises that you ensure it is written into the gestation agreement that the carrier will give birth in Nevada. This allows the intended parents to benefit from Nevada law.
#8 Marriage or domestic partnership of the gestational carrier after execution of the gestational carrier agreement does not affect the validity of the agreement.
#9 “Theoretically, anyone who qualifies via the medical exam and various other requirements can be a surrogate,” McDonnell said. “But the ones that I have seen that worked out the best, with the least problems and the least complications, have been the ones where you’ve got a gestational surrogate who is a family member.” There are numerous successful cases where sisters have done it for sisters or brothers, and mothers have done it for their daughters.
#10 Research lawyers through the Nevada Bar Association, ranking services such as AVVO, and by examining firm websites. There also is an American Academy of Assisted Reproductive Technology Attorneys, of which at least five Nevada-licensed attorneys are members. McDonnell recommends consulting with at least three different attorneys before engaging one to represent you. Do your own research first and go in with questions to see how well versed each lawyer is in this area of law.
• • •
Physical and emotional considerations
While all involved are focused on the child growing in utero, Martin says the OB-GYN must ensure the health of the woman carrying it to term. While women who haven’t given birth before may qualify as surrogates, he thinks the best outcomes are with those who intimately understand what they’re committing to.
“There is an unpredictability in pregnancy. Nobody can ever guarantee the final outcome, whether it’s with their health or with their baby’s health,” Martin said. “Pregnancy physically changes your body and definitely puts it at risk.”
Such changes range from a sharp rise in fluid retention to various forms of cardiac stress, and the potential complications of delivery add considerable complexity to the decision about whether to become a surrogate.
Beyond preparing for the intense physical demands and risks, Martin emphasized that any prospective surrogate should sit down with a psychologist and talk through the emotional impacts.
“It’s such a sacrifice to carry another person’s child,” he said. “You should never take being a surrogate lightly and really understand what it means.”




Join the Discussion:
Check this out for a full explanation of our conversion to the LiveFyre commenting system and instructions on how to sign up for an account.
Full comments policy